Recent comments
Recent posts
 Cancer Research UK Science Update Blog
Cancer Research UK Science Update Blog
- An error has occurred; the feed is probably down. Try again later.
 Psiram/Esowatch
Psiram/Esowatch
- Das Konzept der absconditen Interpaginalität – eine critical hunt for easter eggs
- Psiram Leaks
- Initiative zur Förderung einer gerechten und sachlichen Debatte
- Wohin steuert die GWUP
- #MetooTantra
- Codex Humanus
- Die Deutschen und der Weltfrieden
- Die Metaphysik des Krebsrisikos
- Unabhängige Experten
- Soziologisches zu Cannabis als Medizin
 Respectul Insolence
Respectul Insolence
- An error has occurred; the feed is probably down. Try again later.
 Science-Based Medicine
Science-Based Medicine
- Male and Female Brains are Different
- The Washington Post publishes an advertorial on IV drips
- Dr. Vinay Prasad Pretends to Admit Error: I Was Optimistic That Vaccination Would Halt the Spread of the Virus—I Was Wrong.
- Tattoos Still Won’t Boost Your Immune System
- Binders, fillers and more? What’s all that other stuff in my medicine?
- How To Approach Psychogenic Symptoms
- Dr. Jeffrey Flier: Those Who Express Different Views on Health Equity Should Be Demonized, Not Heard
- A poorly framed article on COVID-19 vaccine injury in the New York Times
- Woke Washing the Pandemic: If You Really Were Progressive, You’d Want Them Infected
- Kava and Liver Damage
 Edzard Ernst
Edzard Ernst
- Yet another case of vertebral artery dissection following cervical spine manipulation
- Skeptics in the Pub
- A comprehensive review on the hepatotoxicity of herbs used in the Indian (Ayush) systems of alternative medicine
- The Effect of Distance Reiki on Anxiety and Test Performance: A Randomized Controlled Trial
- WOW! The German Medical Association bans homeopathy
- Whooping cough is back: please beware of homeopaths, their remedies and their advice!
- Believing in conspiracy theories: The role of emotional granularity and maladaptive emotion regulation
- Health complaints before and after removal of dental amalgam restorations
- Increasing concerns about SCAM research originating from China
- Antibiotic Use in a Neonatal Intensive Care Unit Practicing Integrative Medicine
Blogroll
- A pathologist examines: cancer and fungus
- Alternative Medicine and Cancer
- Ars GeriatriCare (Dutch)
- Cancer Research UK
- Cancer Survival in Europe
- Cryptocheilus medical blog (Dutch)
- Dr. Len's Cancer Blog
- EBM-first: What alternative health practitioners might not tell you
- Medbunker blogspot (Italian)
- My Malignant Melanoma
- Psiram/Esowatch (German)
- Quackwatch
- Science-Based Medicine
Top Posts
Categories
acupuncture
alternative cancer treatment
alternative medicine
antisemitic
baking soda
biologie totale
boosting
breast cancer
cam
Cancer
candida
candida albicans
carcinoma
Caroline Markolin
cat scan
chemo
chemotherapy
chief rabbi
chiropractic
claude sabbah
corinne thos
Dirk Hamer
echinacea
evidence
evidence-based medicine
fungus
garlic
Germanische Neue Medizin
German Medicine
German New Medicine
GNM
götz
Hamer
HBOT
Health fraud
holistic
homeopathy
hoxsey therapy
hulda clarck
images
immune system
iscador
iwan götz
jewish conspiracy
libel
manual therapy
medecine nouvelle
meta medicine
metametrix
metastases
Michaeala Jakubczyk
mistletoe
naturopathy
nouvelle medécine
olivia pilhar
osteopathy
personality
Philosophy of science
positive thinking
psychological aspects and cancer
quackery
rife
Ryke Geerd Hamer
santegod
schneerson
science
Simoncini
sodium bicarbonate
supplements
tony isaacs
total biology
Tullio Simoncini
viscum album
vitamins
zapper

jli,
Thank you so much for this important post! It is very difficult for lay persons to assess the relevance of research on mice and quacks either don’t know themselves or do nothing to enlighten their victims, so I’m very happy you did.
You are welcome. I have been meaning to do this post for some time now. This post on SBM: http://www.sciencebasedmedicine.org/index.php/a-universal-anti-cancer-drug/ gave me the final push.
jli you rock again! Keep up the good work.
Thank you Wilma – And the same to you 🙂
Thank you for this post! I need to send it to the people who emailed me the Burzynski video telling me that I “must watch it!” before I made my decision to do chemo.
Some people just don’t understand.
@ credit card processing goddess
You are welcome. You might also like to show them our post on the testimonials presented in the movie.
Good luck with your treatment.
Thought I’d put this little tid bit just to let you know that there are other cures out there than the excepted norm of promoting Radical treatments like Chemo, Radiation and Radical surgeries
Two Leukemia Patients Healed by Dandelion Tea?
Hopefully this will help some of you non believers see the light ,although thats asking a lot its allways worth a try
Oncologist Dr. Caroline Hamm of the Windsor Regional Hospital had an elderly patient who suffered from myelomonocytic leukemia, a highly aggressive and resistant form of leukemia. When no improvement in her condition resulted after rounds of chemotherapy, the patient began self-administering a natural therapy consisting of dandelion root tea—and even shared the therapy with another patient in the waiting room.
Dr. Hamm was surprised to see that the test results of both patients improved while taking dandelion tea—and both refused further courses of chemotherapy. She then contacted the University of Windsor biochemist Siyaram Pandey, who initially thought that the two patients’ positive results were purely coincidental. Nonetheless, armed with funding provided by the Knights of Columbus Council 9671, he and his students embarked on preliminary research.
The team collected leukemia blood cells from the disposable tissue of nine patients (with their consent). Thereafter, they dug up dandelion roots, formulated a root extract—and applied the extract to leukemia cells in a culture dish.
Dr. Pandey reported that in the presence of the dandelion root extract, the leukemia cells effectively “committed suicide” within 24 hours. “It killed the cells very selectively; it only killed the cancer cells,” said Pandey. “The regular cells were not killed.”
The results were published in the Journal of Ethnopharmacy.
Dandelion Root Extract “Reminds” Cancer Cells to Self-Destruct
At any given moment, cell suicide (called apoptosis) is a process taking place in our body. Whenever cells are no longer needed—or have damaged DNA—they effectively commit suicide.
However, cancer cells evade this process and become resistant to cell death, according to Dr. Pandey. His research attempts to discover how dandelion root extract ‘reminds’ the cancer cells to commit suicide, without killing off the healthy cells.
Scientific Acceptance of Dandelion’s Anti-Cancer Properties
Medical researchers are beginning to regard dandelions as important healing aids in modern phytomedicine. In the past few years, results of clinical research have been published in prestigious publications.
In 2008, the results of a clinical study showing the positive effects of dandelion were published in the International Journal of Oncology. Dandelion leaf tea was shown to decrease breast cancer cells. Researchers tested dandelion leaf tea on prostate cancer cells and found similar results.
The findings on prostate cancer were corroborated by a report published in 2011 by the International Journal of Oncology, which shows that a dietary supplement containing dandelion as one ingredient suppresses the growth of prostate cancer cells.
Dandelion root extract was clinically proven in 2011 to specifically induce apoptosis in chemo-resistant melanoma (a type of skin cancer)—without toxicity to healthy cells.
Native American Medicine and Traditional Chinese Medicine (TCM) have both documented that dandelion extracts are effective treatments for leukemia and breast cancer. These extracts have also been shown to be active against pancreatic cancer cells and colon cancer cells (in vitro, not in humans). There are presently applications for clinical approval to begin trials in humans.
Dandelion root extracts are available as dietary supplements at health food stores and online health retailers.
= = = = = = = = = = =
We have mentioned several times on this blog (and elsewhere), that a lot of useful drugs – including anti cancer drugs – are derived from plants. Beatis even posted this link
The Canadian group isn’t the only ones who is interested in Dandelion. Here is Memorial Sloan Kettering’s take on it
The cases you describe that triggered Caroline Hamm’s attention are not presented as case reports in the medical literature, so I can’t really comment on those. But I have found a recent news media article where she comments on the subject.
The studies you refer to are not clinical studies but pre-clinical studies. Such studies are made to assess whether a clinical study is worth undertaking or not. As explained in the post – You can’t conclude directly from positive preclinical studies to positive effects in the clinical setting. This is why clinical trials are necessary before recommending it as treatment.
This illustrates exactly what is wrong with Big Suppla (BS). Everytime researchers present interesting preclinical data, they turn it into a money spinner for themselves, completely disregarding that it may not turn out to be that miracle they advertise it as. And if the clinical trials fail, they will still claim it is a natural wonder drug, but it is being suppressed by FDA/Big Pharma/Government etc….
Talk about money spinning!!! lets talk about the Myriad of toxic Cancer treatments, Radiation treatments, and Surgeries that wipe out peoples life savings ,and they wind up worse than what they started, because thier immune systems are so devestatded by conventional cancer treatments, their bodies have nothing left to fight with.
If theres a chance that Dandilion Root can help cure my cancer with no side effects I’ll pay the $69.95 US to give it a shot!
Of course you know as well as I, if this Dandilion becomes clinically proven to cure certain types of cancer we both know what will happen…Big Pharma will have the FDA ban it because Big Pharma wont be able to patent it, and make a rediculous amouts of money.
So as you stated the Big Suppla (BS ) as you put it, will try and milk it proven or not, maybe, maybe not. I can gaurantee you this though, regardless whether proven or not the FDA will do everything in their power to make it go away.
Having cancer and having it treated is tough – no argument there. But remember that in most of the civilised world, conventional cancer treatment is free (Taxpayer funded). Treating cancer costs oncology departments money. A safe cheap and effective drug is more than welcome among conventional doctors. So the financial argument is not valid. You have an upcoming election. Why not go and campaign for people who are in favour of socialised medicine?
It is a fact that countless of wonderful people are still with us today because of conventional cancer treatments. Be careful not to confuse deaths due to adverse events with preventable deaths. Failing to treat curable cancers with chemotherapy would reduce the number of deaths due to complications of chemotherapy. But the number of deaths due to cancer will rise, and those people who did not die from a chemotherapy related complication will still die.
A few studies have been done to see what happens to patients who chose alternative therapy instead of conventional treatment. These studies show that the risk of progression/death significantly increases – most notably in those who refuse surgery, but also in those who refuse additional radio-chemotherapy.
You can read the summaries of those studies here:
http://www.ncbi.nlm.nih.gov/pubmed/16978951
http://www.ncbi.nlm.nih.gov/pubmed/21225354
History tells us otherwise. I linked to a site listing numerous patented drugs derived from plant substances. Here it is: http://chemistry.about.com/library/weekly/aa061403a.htm
Besides FDA have no juristiction outside US.
Hopefully you have been given enough food for thought so that you will begin to see the light. I realize that’s asking a lot, but at least I have tried.
There are well known cures for cancer and yet they suppress them, that is sad. I guess you can’t make money on healthy people!
There are well-known quack treatments for cancer and yet they are being sold widely on the internet, that is not just sad, it is downright criminal. No one has ever been cured of cancer with alternative treatments. Quackery is despicable and cancer quackery is the most despicable of them all.
Pingback: For those who have cancer, have any of you tried using cannabis? If so what were the results? - medical research papers
Quack?
http://engr.arizona.edu/news/story.php?id=429
My favorite paragraph:
“Drinking baking soda has been proven to reduce or eliminate the spread of breast cancer to the lungs, brain and bone”
The article is correct in that (many) cancers produce lactic acid, thus creating a local acidic environment. And this helps in spreading the tumour. But the part that reads:
suggests that the professor got it wrong, or that she believes that studies in experimental rodents can be directly translated into effects in the human clinical setting. The study I believe she draws her conclusion from is discussed here.
Thank you, Jill, I appreciate the post and the response.
I don’t claim to know it all or much about the medicine or chemistry. What I do know, though, that I measured my pH (urine) with a strip before drinking a glass of water with a teaspoon of baking soda and after. The before measurement was ~5, after ~8. Not sure what you meant by stating that “the professor got it wrong”, but humans can and do change their pH all the time (it is a known fact that a vegetarian diet is associated with more alkaline pH). If you are really interested, you can try it yourself, pH measurement strips are sold in pharmacies (try CVS and Walgreens).
Of course, this doesn’t mean that baking soda is a miracle cure, that would be too good to be true. But after starting drinking it twice a day I have lot more energy and the pain that I had for almost two months is almost gone. Interpret it as you wish, I just hope that it continues to help me feel better and that maybe, just maybe, it will slow down my tumors enough to squeeze several more good years.
In general, I applaud your trust in modern traditional medicine. The progress in treating cancers (many of them, at least) is undisputable and very real. But you do have to admit that:
1) They still don’t have answers to very basic questions: what causes cancer, why some people get it while others don’t, etc.
2) That the medicine in the US and most of the modern world is a profit driven industry and as such it is full of conflicts of interests.
3) And that there are very significant variations of the cancer rates around the world with the developed countries being afflicted disproportionately higher and that those countries that adopt the western life style see a dramatic increase of those rates shortly after.
We are a long way to go before cancer becomes a treatable and manageable disease. Until then, I personally would welcome anything that helps, for real or in imagination only.
Good luck to us all.
More “quackery”: http://www.sciencedaily.com/releases/2007/09/070910132848.htm
Those profs must have gotten something wrong, too 🙂
Even more:
http://www.canadianmedicaljournal.ca/content/174/7/937.full
This is because of the mechanisms that work to maintain a stable pH in the body.
The body is by nature slightly alkaline with a pH around 7,4. Various regulatory mechanisms in your body work to maintain a stable slightly alkaline pH. This is necessary for the body to function properly.
So one really can’t (and shouldn’t wish one could) make the body more alkaline/acidic. The rumours that claim that altering the body pH will prevent/cure cancer, and that this can be achieved through certain diets or supplements are false. The changes in urinary pH are simply a result of the body’s regulatory mechanisms, where excess acid/base is eliminated through the kidneys.
Here is a good blog post elaborating on this subject: http://sciencebasedpharmacy.wordpress.com/2009/11/13/your-urine-is-not-a-window-to-your-body-ph-balancing-a-failed-hypothesis/
We have a lot of knowledge about the events that happen to normal cells which turn them into cancerous cells. If you are interested, I can recommend this site: http://www.insidecancer.org/
I work in a taxpayer financed healthcare system (I am a pathologist). Expensive treatments put strains on our budgets. We would more than welcome an effective and inexpensive cancer treatment. Not all cancer research is funded by the pharmaceutical industry (I do taxpayer funded cancer research). And adverts from pharmaceutical companies are not the only source of information that oncologists use.
You should also understand that every cured patient is a success for the treating doctor. In a profit based health care system, the doctors with the highest cure rates would receive the most patients and consequently score higher profit.
If other causes of death are eliminated, more people will live long enough to get cancer.
British Journal of cancer recently published an issue on cancer attributable to lifestyle and environmental factors: http://www.nature.com/bjc/journal/v105/n2s/index.html The researchers found that about 43% of new cancers in UK could be attributed to such factors.
I don’t share your pessimism. Today more than 50% of all cancers are cured through conventional treatment. Outlooks for individual cancer patients are far better today than they were 20 years ago. And I am absolutely confident that they will be even better in 20 years from now. All thanks research and evidence based medicine.
You might like to take a look at how progression has been made in the treatment of childhood cancers: http://info.cancerresearchuk.org/cancerstats/childhoodcancer/survival/ Children are not part in screening programs, so what you see is not just a consequence of earlier detection.
If you read the article again, you should be able to find the part where it says:
This is far from quackery. The statement is in fact the point of this blog post.
EDIT TO ADD:
I found the original research paper: http://www.sciencedirect.com/science/article/pii/S1535610807002334
You might like to take a look at figure 5, and form your own opinion if you think that the results support that Vitamin C would be an effective treatment of all cancers.
It is quackery to use the three reported cases in the article as proof that Vitamin C is a cure of all cancers.
I am guessing that you haven’t actually read the paper, but accepted it as proof by someone who peddles Vitamin C as cancer treatment. But if you do read the paper yourself you will find the following:
Patient nr. 1:
Had a renal cell carcinoma. This is important, because metastasis from renal cell carcinoma is one of the most frequently reported undergoing spontaneous regression. In addition the patient used other types of alternative therapy.
So there are two other possibilities than Vitamin C:
1) Spontaneous regression – Biologically plausible given the cancer type.
2) Other types of alternative therapy (unlikely, but we can’t really know)
A few years later the patient developed small cell lung cancer, and vitamin C weren’t helpful at all then.
Patient nr. 2:
Had a “Transurethral resection” of a bladder cancer (TURB), and declined additional conventional treatment. Instead he had Vitamin C and other types of alterative therapy.
So again – there are two other possible expalanations than Vitamin C:
1) The TURB was sufficient (The article reports a 20% cure rate of T2 bladder cancer through TURB alone)
2) Other types of alternative therapy (unlikely, but we can’t really know)
Patient nr. 3
The patient was diagnosed with a “diffuse large cell B lymphoma” and received radio therapy. Instead of additional chemotherapy she had Vitamin C and other types of alternative therapy. Subsequently the patient had other enlarged or palpable lymphnodes, but they were never confirmed histologically to be lymphoma recurrences.
So again we have two other possible explanations than Vitamin C:
1) The radiotherapy was sufficient
2) Other types of alternative therapy (unlikely, but we can’t really know)
EDIT TO ADD:
It turns out that David Gorski from Science Based Medicine analysed this study back in 2008. In his blog post he also analysed another experimental study, and recapitulated the history of the Vitamin C fuss. If you are interested I think his post is highly recommendable, so here is the link: http://www.sciencebasedmedicine.org/index.php/high-dose-vitamin-c-and-cancer-has-linus-pauling-been-vindicated/
Pingback: De ware geschiedenis van Softenon « Cryptocheilus Weblog
I think the significant conclusion to take here is that Cannabis is a very promising area of research for cancer treatment, and while it is a very good point to bring up animal / rat testing does not extrapolate up to humans all the time, the world needs to actually start moving to human trials. ESPECIALLY considering that chemo, radiation, and surgery are the only real widely accepted treatments and they are all very destructive to your body, especially chemo. My mom has been fighting lung cancer and we have almost lost everything because chemo has made her so weak that she had to leave her job. She almost died because she was too weak to get out of bed and eat (not because of the effects of the cancer!). This is not the treatment I want to see for my children and grand children.
Once the world pulls their head out of their ass and legalizes research on Cannabis, which there is nearly ZERO risk to run trials in with humans (because your body contains natural Cannabinoids and was made to receive them!) we can get an answer to this question. But as long as “cancer research uk” continues with attitudes like stated in their article:
“Why don’t you campaign for cannabis to be legalized?”
As things currently stand, cannabis is classified as a class B drug in the UK, meaning that it is illegal to possess or supply it.
It is not for Cancer Research UK to comment on the legal status of cannabis, its use or abuse as a recreational drug, or its medical use in any other diseases. But we are supportive of properly conducted scientific research that could benefit cancer patients.”
That’s unfortunate. So basically “It’s illegal so we’re gonna stay away from it for now. And it’s not really promising anyway so don’t want people to miss out on chemo!” And they go on to say things like :”And there’s certainly no evidence that ‘street’ cannabis can treat cancer.” WHAT? you’re saying that grown Cannabis sold on the street is somehow different and there’s no evidence? “street” cannabis contains all the other compounds as… well.. are you comparing it to hemp oil? Just ask your dealer for an indica strain, as these have a high amount of CBD the main anti-cancer compound (although others do have effect see below)
Let’s make a list:
– THC and THC-V and CBD (Cannabidol) have been shown in lab and animal trials to 1) kill cancer cells, 2) reduce blood flow to tumors, and 3) trails have tested, by artifically reducing the rat’s natural cannabinoids in their body, they become fraught with cancer.. suggesting that the endocannabinoid system’s purpose in part is to PREVENT cancer. This is screaming “TAKE ME TO HUMAN TRIALS”.
– Because of our natural endocannabinoid system, cannabis is a near zero risk drug because it is impossible to lethally overdose, does not cause withdrawal symptoms since the compounds are fat soluble: they release small amounts back in the blood stream for a few days after ingested. Furthermore, it does not fit the scientific definition of an addictive substance.
– Cannabis may be an effective treatment for brain cancer. Since the compounds are fat soluble and oily, they pass the blood brain barrier (which chemo CANNOT), so we can conclude if it’s effective at treating cancer in humans then we have a natural, non-destructive alternative to chemo and radiation.
– It’s already been proven over and over that Cannabis is a good treatment of many nervous system diseases such as MS, Lupus, Arthritis, etc. You can’t deny that through the “not enough clinical trials” research line of thinking. This is why big pharma is scared! (Read below >>)
– Despite what cancer research UK says, yes big pharma does not want cannabis to get out as a possible cure. Saying that cannabis can’t be touted as a cure because it hasn’t been “brought to patients [is] through proper research using quality-controlled, safe, legal, pharmaceutical grade preparations containing known dosages of the drugs.” is a cop-out. First of all, cannabis CAN be administered in safe pharmaceutical grade preperations (tinctures, oils, vaporizers) making that line a straight out LIE, and secondly… is that why chemo and radiation are accepted as forms of treatment? Even though they are destructive to your entire body, as WELL as cancer, it’s ok because it has been tested a little more? Did you know chemo leads to hearing loss, and baldness?
Please. Enough of this rhetoric. I think it’s interesting that my google query “if marijuana is the cure for cancer why does no one want you to know” today brought up this page and cancer research uk and you link to that page. And both try to push reasonable doubt on the substance. Instead of saying “Oh well it hasn’t been thoroughly tested in humans enough”, how about we band together to END cannabis prohibition and make PROGRESS! Instead I guess people at cancer research uk like to try and shed so much doubt on the subject it doesn’t leave much interest to pursue it.
@ Izzy Rallins
Personally I think the blogpost on cancerresearch.uk is a good and well balanced post. This blog is based in The Netherlands (I am Danish though) where cannabis is legal, so the legal aspects is really not an issue here.
Research into anti-cancer capabilities is no different than resaerch into anti-cancer capabilities of other plants. There are more than 100 patented (and important) drugs that are derived from plants: http://chemistry.about.com/gi/dynamic/offsite.htm?site=http://www.rain-tree.com/plantdrugs.htm
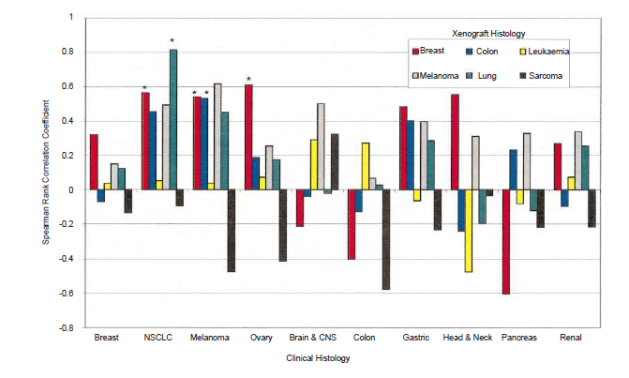
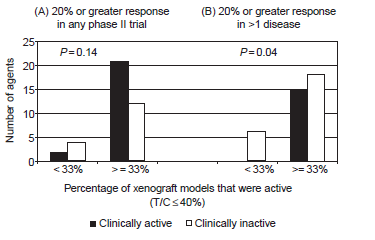
As explained in the post, THC only reduced tumour size in mice by 50 %. This is simply not good enough to make pharmaceutical companies (or independent reseachers) interested. Given the poor correlation between substances that reduce tumour size by at least 60 % and results in clinical trials, I understand why they want to spend their drug development funds elsewhere.
Pingback: Sugar depleted diet is not a useful cancer cure | Anaximperator blog
Pingback: Does research at University of Arizona show that drinking baking soda cures cancer ?? | Anaximperator blog
I think that another important fact we always overlook is the fact that humans are one of five mammals (the other four are prime apes in our human family or close) that can not produce their own Vitamin C.
Most other mammals like mice, rats, rabbits, (used for research) can make their own Vitamin C.
Now we find that high doses of injected Vitamin C can be beneficial and can help cure certain Cancers. So the testing done on any medication using rodents is flawed from the onset.
The Rodents have, I would think a stronger immune system and may be more resilient to infections, diseases, and viruses
Vitamin C Protocol.
We do have some interesting case reports and we also have results from phase 1 studies. We don’t have results from randomised controlled trials, so we don’t really know how useful it may be. But research is ongoing.
Hi! I read a 25-page in vitro and “in mus” experiments with graviola – and although it seemed to kill everything, one thing kept worrying me: if the supposed mechanism of action is inhibition of mitochondrial complex 1, isn’t it terribly dangerous, leading to many kinds of neuromuscular disorders although graviola supporters say the action is cancer cell specific. The poor mice didn’t develop deficiency symptoms of course because they were slaughtered after 35 of treatment. (I never even dream of believing other than clinical trials when treating patients of course but I wonder if graviola extract is at all safe as a supplement…)
***missed a few words at the beginning***’ spank me **** a 25-page report on etc.
Toxic effects of Graviola in mice attributable destruction of dopaminergic nerve cells (such as lowered blood pressure, decreased heart activity, apatia, nausea/vomiting etc.) have been reported.
It should also be mentioned, that scientists aren’t against looking into useful substances in plants. Here is a list of many plant derived important drugs: http://www.rain-tree.com/plantdrugs.htm But as of today, a Graviola derived drug is not among them.
I prescribe plant-derived drugs almost daily – taxanes, vinca alkaloids, opioids… I keep telling some pro-quackery patients that if chaga mushroom is some day proven safe and effective it will be included in the treatment protocols but they just don’t seem to get the message.
Pingback: Alternativ behandling af kræft virker ikke | Alternativ behandling for kræft
Pingback: Cannabis er desværre ikke den ultimative kræftkur | Alternativ behandling af kræft
Pingback: Mistelten og kræft | Alternativ behandling af kræft