
In the Dutch Medical Journal, authors from the University Hospital St. Radboud in Nijmegen, Netherlands, report a tragic case history of an infant dying after being treated by a craniosacral therapist.
Deceased infant after “craniosacral manipulations” of neck and vertebral column
(Transl Beatis)
A formerly healthy, three-month-old girl died after manipulation of the neck and the vertebral column by a so called “craniosacral therapist.” During continued and deep bending of the neck, the patient developed incontinence of faeces, atonia and respiratory arrest followed by aystolia. Based on findings at the physical examination of the body, an additional MRI examination and the autopsy, it is likely that the cause of death was a local neurovascular or a mechanic respiratory-induced problem. This is the second report of infant death after forced manipulation of the neck. As long as there is no scientific evidence for the efficacy and safety of forced manipulation of the neck and the vertebral column, we advise against this treatment for newborns and infants.
Clinical Practice
Manipulations of the neck and the vertebral column are applied world-wide for very different symptoms. Although there is no conclusive evidence for the usefulness of this technique (1), it is also used with infants, to counteract excessive crying, motoric unrest and an asymmetrical positional preference of the head.
In this article, we describe the decease of an infant, following forced manipulations of the neck and the vertebral column. For this we made use of the hetero anamnesis of the parents who were present at this procedure.
Case history
Patient A was a three-month-old, healthy girl. Because their child exhibited mild motor unrest, the parents contacted a so-called “craniosacral” therapist who, after a short introductory interview, started administering the craniosacral therapy. He placed the child on her back on a changing mat, after which he palpated the neck and the skull. The patient cried vehemently at this. Then she was turned to her right side and a deep bending of the vertebral column was applied at 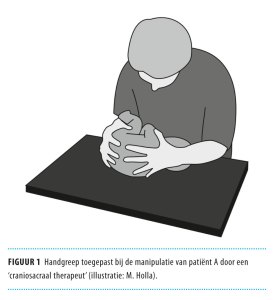 which the chin touched the chest, as shown in figure 1. After the vertebral column was bent deeply in this manner during several minutes, the child lost faeces and several loud intakes of breath were clearly audible. The therapist interpreted this as a deep sleep, which he said was normal during the treatment. After about 10 minutes the girl was placed on her back and blue discolouration of the lips was apparent. The child was limp now and did not react to touching. The father started mouth-to-mouth resuscitation. Alerted ambulance personnel on arrival saw a deceased infant with asystolia. One hour after the reanimation had started, the patient showed a heart rate again with palpable pulsations. On arrival at the hospital, an intubated infant was seen with a body temperature of 32°C, a heart rate of 120 beats per minute and a bloodpressure of 60/30 mmHg. Physical examination of heart, lungs, abdomen and extremities showed no particularities. Without sedation the Glasgow Coma Score was E1M1Vtube. No abnormalities were seen in conventional radiology examination of the torso and the extremities. There was overall hypotonia, while tendon reflexes, cornea reflexes, oculocephalic reflexes and coughing reflexes were absent. A CT scan of the brain, the neck and the vertebral column showed no abnormalities, recent hemorrhages, fractures or dislocations. The MRI examination of the head, the neck and the vertebral column showed abnormalities within the pons and mesencephalon, corresponding with ischemia in the vertebrobasilar artery basin. Especially in the cervical part of the spinal cord and medulla oblongata signal abnormalities were seen (figure 2).
which the chin touched the chest, as shown in figure 1. After the vertebral column was bent deeply in this manner during several minutes, the child lost faeces and several loud intakes of breath were clearly audible. The therapist interpreted this as a deep sleep, which he said was normal during the treatment. After about 10 minutes the girl was placed on her back and blue discolouration of the lips was apparent. The child was limp now and did not react to touching. The father started mouth-to-mouth resuscitation. Alerted ambulance personnel on arrival saw a deceased infant with asystolia. One hour after the reanimation had started, the patient showed a heart rate again with palpable pulsations. On arrival at the hospital, an intubated infant was seen with a body temperature of 32°C, a heart rate of 120 beats per minute and a bloodpressure of 60/30 mmHg. Physical examination of heart, lungs, abdomen and extremities showed no particularities. Without sedation the Glasgow Coma Score was E1M1Vtube. No abnormalities were seen in conventional radiology examination of the torso and the extremities. There was overall hypotonia, while tendon reflexes, cornea reflexes, oculocephalic reflexes and coughing reflexes were absent. A CT scan of the brain, the neck and the vertebral column showed no abnormalities, recent hemorrhages, fractures or dislocations. The MRI examination of the head, the neck and the vertebral column showed abnormalities within the pons and mesencephalon, corresponding with ischemia in the vertebrobasilar artery basin. Especially in the cervical part of the spinal cord and medulla oblongata signal abnormalities were seen (figure 2). 
Radiological differential diagnosis of images of the cervical spine could point to direct trauma or overall asphyxia.
The cerebrum was oedematose, non-abnormal basal nuclei. No indications were found for dissection of the neck arteries, congenital anomalies, fractures, band injuries or haemorrhaging. Laboratory testing showed a metabolic acidosis with a pH of 6.62 and an elevated lactate concentration: 20 mmol / l (reference values: 0,5-1,7), and abnormal kidney and liver functions. Microbiological examination showed no indications of of a bacterial or viral infection. The ECG showed no abnormalities, the QT-time in particular was not extended. Ultrasound examination showed non-abnormal anatomical characteristics of the heart and a good left ventrical function. In fundoscopy, sharply defined papillae were seen on both sides, without bleeding in the retina.
While in the department of Pediatric Intensive Care, the infant developed further signs of progressive multi-organ failure and 12 hours after the manipulation, continued spontaneous breathing activity, brainstem reflexes and tendon reflexes remained absent. After multidisciplinary consultation we decided to stop the treatment. The girl died a few minutes later.
In the autopsy by the Dutch Forensic Institute, recent infarctions were seen in the spleen and the heart, corresponding with lack of oxygen and multi-organ failure. The brain showed signs of hypoxic encephalopathy. On a number of levels in the spinal cord, subtle axonal abnormalities were visible, which could have arisen because of hypoxia or stretching of the vertebral column. There were no indications of congenital deformities, organ abnormalities or infections.
Consideration
In the death of this patient the following factors may have played a role.
Neurological causes
During manipulation of the neck, the cervical spine may be wedged by the vertebral column. As the skeleton of infants consists mainly of cartilage, this may occur without radiologically visible abnormalities of the spine (2).
Temporary irritation or wedging of the myelum can result in a neurogenic bradycardia with apnoea.
Vegetative reactions, including apnoea and flushing of the face were seen earlier in 53% of infants during manipulations (3).
In another study, reduced heart rate after manipulation of the neck was observed in 40% of the infants. Children younger than 3 months developed more serious bradicardias; 12% of the children had apnoea (4).
Vascular causes
During manipulation of the neck indirect neurogenic damage can arise because of injury or wedging of the A vertebralis (5). Ischemia of the myelum can generate symptoms of a high spinal cord injury (6).
Respiratory causes
A forced curved position of the neck may cause obstruction of the upper respiratory tract. Infants are more sensitive to airway obstruction than adults because of the relatively large tongue, narrower airways, weaker cartilage and the anterior position of the larynx (7). Also, thoracic breathing can be hampered by the curved posture.
Other causes
On the basis of further investigation in our case, no signs of an infection, congenital abnormalities, cardiac or gastro-intestinal disorders were found. Given the relationship between spinal manipulation and the emergence of symptoms, a causal relationship seemed plausible.
Conclusion
Next to well-known risks of manipulation of the spine in adults (8), in 2005 the risks of spinal manipulation in infants were already pointed out. To this date, the decease of one other infant after manipulation of the vertebral column has been described (9). In that case the head of the infant had been rotated with some force. Our case demonstrates that also with a forced deep bending of the neck fatal complications may arise. As long as there is no scientific evidence for the efficacy and safety of forced manipulation of the spine, we advise against this treatment for infants.
The events of this case history prompted the public prosecution office to start an investigaton of the case.
Learning points
- There is no scientific eviedence of the efficacy of forced manipulations of the vertebral column in children.
- Forced manipulation of the vertebral column in a child can lead to serious complications.
University Medical Centre St Radboud, Nijmegen.
Dept. of Orthopedic Surgery: Dr. M. Holla, orthopedic surgeon.
Dept. of Pediatric Intensive Care: Dr. M.M. Ijland, pediatrician, fellow pediatric intensive care; Dr. C.W.M. Verlaat, pediatric intensivist.
Dept. of Radiology: Dr. A.M. van der Vliet, neuroradiologist.
Dept. of Surgery: Dr. M. Edwards, surgeon.
Literature
| 1 |
Brand PLP, Engelbert RHH, Helders PJM, Offringa M. Systematisch literatuuronderzoek naar de effecten van behandeling bij zuigelingen met ‘kopgewrichteninvloed bij storingen in de symmetrie’ (‘KISS-syndroom’). Ned Tijdschr Geneeskd. 2005;149:703-7. |
| 2 |
Pang D, Wilberger JE Jr. Spinal cord injury without radiographic abnormalities in children. J Neurosurg. 1982;57:114-29. |
| 3 |
Koch LE, Biedermann H, Saternus KS. High cervical stress and apnoea. Forensic Sci Int. 1998;97:1-9. |
| 4 |
Koch LE, Koch H, Graumann-Brunnt S, Stolle D, Ramirez JM, Saternus KS. Heart rate changes in response to mild mechanical irritation of the high cervical spinal cord region. Forensic Sci Int. 2002;128:168-76. |
| 5 |
Kuitwaard K, Flach HZ, van Kooten F. Dubbelzijdige A.-vertebralisdissectie tijdens chiropraxiebehandeling. Ned Tijdschr Geneeskd. 2008;152:2464-9. |
| 6 |
Brand MC. Part 1: recognizing neonatal spinal cord injury. Adv Neonatal Care. 2006;6:15-24. |
| 7 |
Turner NM, van Vught AJ. Advanced paediatric life support. 2e dr. Maarssen: Elsevier Gezondheidszorg; 2006. |
| 8 |
Ernst E. Adverse effects of spinal manipulation: a systematic review. J R Soc Med. 2007;100:330-8. |
| 9 |
Jacobi G, Riepert Th, Kieslich M, Bohl J. Über einen Todesfall während der Physiotherapie nach Vojta bei einem drei Monate alten Säugling. Klin Padiatr. 2001;213:76-8. |
Reference:
Micha Holla, Marloes M. IJland et al. Ned Tijdschr Geneeskd, 2009
Comments
Members of the Dutch professional society of manual therapists:
May 8, 2009
Despite the fact that the authors have been very careful in their search for an explanation for the cause of death of the deceased infant, they do not succeed in establishing the likelihood of a causal relationship between this death and the therapy that was performed. Less careful is the way in which they have formulated their conclusion. On the basis of no more than an assumption, a negative advice is given on a therapy. Holla et al are neither qualified nor competent to do so. This seems inappropriate to us.
Should there appear to be a causal relationship however, then we can agree with the authors that possibly the therapist acted incompetently or negligently. This would be uncommon however and no reason to advice against or reject a therapy as such. In the medical world complications occur regularly in all disciplines and when negligence is established, measures are taken against individuals and institutions and not against an entire discipline.
Holle et al conclude that this is the second report of the decease of an infant after forced manipulation of the neck. If there has actually been a spinal manipulation as described in the nomenclatura of the manual therapist, then the acting craniosacral therapist has crossed the boundaries of his profession. The same applies to the other case which is referred to, where a children’s physiotherapist went outside the competence of her own field and applied manual therapy, for which she was neither authorized nor qualified, with disastrous consequences.
Holla et al had better call for the manipulation of infants by manual therapists only. Within the field of manual therapy, infants with asymmetrical head turning (excessive crying, KISS children) are treated. Training is done by the European Workgroup for Manual Medicine (EWMM). The EWMM manages a specialist register and initiates research. Treatment data have been registered since 2006 and on the basis of that we can report that (KISS) manual therapists have treated more than 21,000 infants in 66,239 treatment sessions without any complications. At the Faculty of Epidemiology of Maastricht University a cohort study with a control group is in preparation, in which the efficacy of manual treatment in asymmetrical infants will be studied.
Lastly, we would like to point out that a specialised manual therapist would never apply manipulations in the treatment of infants, let alone forced manipulations of which Holla et al speak. Rather, the description should read: targeted mobilizing impulse of very low intensity.
Practice for MT & FT, Boxmeer, the Netherlands
Eric Saedt & Bé van der Woude, manual therapists and members of the EWMM Nederland
Dutch craniosacral therapists:
The Nederlandse Cranio Sacraal Vereniging (Dutch CranioSacral Association) does not recognise this manipulation. According to a spokeswoman, craniosacral therapy tries to solve physical and psychological problems by “following the movement of the brain fluid with the hands, leading to a relaxation of the body.”
The therapist is not known at the professional association. The spokeswoman says that this could indicate that the practitioner isn’t certified.
Register CranioSacraal therapie Nederland (RCN), Velp; Verenigingen voor Upledger CranioSacraal therapie Nederland en Duitsland (Societies for Upledger CST Netherlands and Germany); Upledger Instituten Nederland, Duitsland en België (Upledger Institutes Netherlands, Gemany and Belgium)
Karin van Deelen-Wortman, secretaris RCN (Secretary RCN)
May 25, 2009
(1)The actual cause of death is unclear. Two possible causes are mentioned of which a direct link to the decease is not proven. The MRI images could be consistent with a “direct trauma or with overall asphyxia” and the autopsy report mentions “subtle axonal deviations which could have been caused by hypoxia or stretching of the spinal cord.”
In the article a causal relation is assumed between spinal manipulation and/or forced deep bending of the neck and the occurence of the symptoms. This is premature and wants further research and discussion, especially with regard to the following:
- the case history is based completely on the findings of the hospital and the heteroamnesis of the parents. The report of the therapist who treated the infant was not used to link actions and symptoms to a time line.
- A “direct trauma or stretching of the spinal cord” as the cause of death was not demonstrated. “Overall asphyxia with hypoxia” or other causes were not excluded.
- That the patient was healthy and without injuries before the treatment was not demonstrated.
- That the alleged mechanical force was applied during and because of the treatment was not demonstrated.
- The life saving and stabilizing measures may have contributed to the results of the MRI exam and the autopsy.
(2) It is unclear what is meant by “forced manipulation” and “forced deep bending.” It was not even shown that such actions were used during the treatment. The relation between such manipulations and CST is unjustly made.
The assumptions in this case history are premature. In our opinion, further research and discussion are necessary.
Reply from the MDs treating the infant:
May 26, 2009
The incidents during the treatment were described by both parents. At numerous moments they have given coherent and reproducible description of the incident. We see no reason to doubt their statements. Due to medical confidentiality we have not been in contact with the therapist. No public statement of the therapist is available and we have not received a reaction from the therapist.
Apart from mild motor unrest the parents described no symptoms indicating earlier illness or serious afflictions. The GP’s medical contained nothing remarkable either. Directly prior to the treatment, the child was awake, showed normal movements of arms and legs and reacted well to external stimuli. With the help of extended examinations and autopsy no indications were found that the child had been ill previously or had any congenital defects. Therefore we speak of a newborn being healthy before treatment.
Both parents have described that the therapist actively bent the girls head, neck and beck with both hands. This was done with such force that the chin touched the breast. Therefore we speak of a forced bending of the neck. All the time during the reanimation, the neck and the vertebral column were completely immobilized by the medical team. Because of the accident mechanism, in the hospital the neck and the vertebral column were not bent again. The axonal damage of the spinal cord consistent with stretching, which was observed during the autopsy, therefore cannot be explained by the life saving measures that were delivered. Also, the distinctive features of lack of oxygen of the brain and the organs cannot be reduced to the life saving and life stabilizing actions. On the contrary, these actions are specifically aimed to supply the patient with oxygen.
In our article we describe various pathophysiological mechanisms as the possible cause for the symptoms that were observed. Which of these is responsible for the fatal outcome remains unclear. The fact remains however that the serious symptoms which eventually led to the death of a newborn girl occurred during the deeply bent position of the neck and the vertebral column. The findings of the additional examination and the autopsy are consistent with previous over-stretching of the spinal cord, cardiac arrest and respiratory problems and confirm the causal relation between the forced position and the symptoms described.
We find it worrying that the people who perform these manipulations deny or do not recognize the relation between forced bending of the vertebras and the occurrence of serious symptoms. With this case report we hope to prevent another incident like this.
University Medical Centre St Radboud, Nijmegen.
Micha Holla, Marloes IJland, Michael Edwards, Ton van der Vliet & Carin Verlaat.
 Cancer Research UK Science Update Blog
Cancer Research UK Science Update Blog Psiram/Esowatch
Psiram/Esowatch Respectul Insolence
Respectul Insolence Science-Based Medicine
Science-Based Medicine Edzard Ernst
Edzard Ernst
 which the chin touched the chest, as shown in figure 1. After the vertebral column was bent deeply in this manner during several minutes, the child lost faeces and several loud intakes of breath were clearly audible. The therapist interpreted this as a deep sleep, which he said was normal during the treatment. After about 10 minutes the girl was placed on her back and blue discolouration of the lips was apparent. The child was limp now and did not react to touching. The father started mouth-to-mouth resuscitation. Alerted ambulance personnel on arrival saw a deceased infant with asystolia. One hour after the reanimation had started, the patient showed a heart rate again with palpable pulsations. On arrival at the hospital, an intubated infant was seen with a body temperature of 32°C, a heart rate of 120 beats per minute and a bloodpressure of 60/30 mmHg. Physical examination of heart, lungs, abdomen and extremities showed no particularities. Without sedation the Glasgow Coma Score was E1M1Vtube. No abnormalities were seen in conventional radiology examination of the torso and the extremities. There was overall hypotonia, while tendon reflexes, cornea reflexes, oculocephalic reflexes and coughing reflexes were absent. A CT scan of the brain, the neck and the vertebral column showed no abnormalities, recent hemorrhages, fractures or dislocations. The MRI examination of the head, the neck and the vertebral column showed abnormalities within the pons and mesencephalon, corresponding with ischemia in the vertebrobasilar artery basin. Especially in the cervical part of the spinal cord and medulla oblongata signal abnormalities were seen (figure 2).
which the chin touched the chest, as shown in figure 1. After the vertebral column was bent deeply in this manner during several minutes, the child lost faeces and several loud intakes of breath were clearly audible. The therapist interpreted this as a deep sleep, which he said was normal during the treatment. After about 10 minutes the girl was placed on her back and blue discolouration of the lips was apparent. The child was limp now and did not react to touching. The father started mouth-to-mouth resuscitation. Alerted ambulance personnel on arrival saw a deceased infant with asystolia. One hour after the reanimation had started, the patient showed a heart rate again with palpable pulsations. On arrival at the hospital, an intubated infant was seen with a body temperature of 32°C, a heart rate of 120 beats per minute and a bloodpressure of 60/30 mmHg. Physical examination of heart, lungs, abdomen and extremities showed no particularities. Without sedation the Glasgow Coma Score was E1M1Vtube. No abnormalities were seen in conventional radiology examination of the torso and the extremities. There was overall hypotonia, while tendon reflexes, cornea reflexes, oculocephalic reflexes and coughing reflexes were absent. A CT scan of the brain, the neck and the vertebral column showed no abnormalities, recent hemorrhages, fractures or dislocations. The MRI examination of the head, the neck and the vertebral column showed abnormalities within the pons and mesencephalon, corresponding with ischemia in the vertebrobasilar artery basin. Especially in the cervical part of the spinal cord and medulla oblongata signal abnormalities were seen (figure 2). 
I have seen this article a couple of times now. There is no CST training that includes forceful manipulation of the vertebrae as part of the training. CST is based on an extremely gentle touch. Any manipulation would come from an osteopathic or chiropractic background. I have treated hundreds of newborns with CranioSacral Therapy and only had positive results.
Be that as it may, the person delivering this treatment called himself a craniosacral therapist.
I hear you on that and if they were doing manipulations and calling it CST, that is wrong. I just thing we need to avoid giving all CranioSacral therapists and the therapy a bad name. I just wanted to be clear that CST as it is taught, is very gentle and safe.
Should manipulations be done on a baby’s neck? In my opinion..not at all. I believe it takes until around age 4 for the Atlas to become a solid bone.
Nice chatting with you.
In the articles figure 1 http://www.ntvg.nl/jaargangen/2009/jpg/A290_F1.jpg it is illustrated what was done. It doesn´t look like chiropractic style manipulation to me. Don´t know so much about CST to tell if some CST variety would apply a treatment like that. On your site you refer to a John Upledger as the inventor of CST. I know of a William G Sutherland who invented it back in the 1930s. Perhaps you could tell us if both CST systems are the same, or if they differ in anyway.
Perhaps you could also comment on these two incidents of CST-treatments going wrong: http://whatstheharm.net/craniosacraltherapy.html
Been doing some googling on craniosacral therapy and what it is used for and found this:
http://www.sussexholistictherapy.co.uk/craniosacral.html
Among other things, they claim: “Using Upledger CranioSacral Therapy it is possible for you to identify the probable reason for the presence of the cancer. This may be because of external sources such as toxins or radiation or it may be from an emotional conflict within your body.”
This kind of completely unproven, holistic twaddle gives me instant rash. Sorry.
So in looking through my site I cannot find the place where I say he invented it. On the very first page I say that he is the developer of it. Developing something does not mean inventing it. Of course Dr. Sutherland came up with it. Dr. Upledger has been the main proponent of the work for a very long time. He has been credited by countless people as bring the therapy into the mainstream. There are many others who have also developed their own brand of CST.
As to the two issues you site. One is Cranial Osteopathy, not CST. I cannot comment on that as I am not trained in it.
The second seems to be an issue of a chiropractor convincing person with epilepsy to go off their meds. Even the article talks about the medication issue. Not sure what that has to do with the therapy aspect of CST. There is a giant leap taken in the article when talking about meninges. It is assumed that they are talking about CST. There is a form of chiropractic called Network Chiropractic that focuses on releasing the tension in the Meninges. How do you know they were not talking about that? What this person did is just incredibly bad judgement, and I am glad something happened as a result.
I’m not going to comment on another clinics words. Have I worked with people who have cancer? Yes. Have some of those people had incredible emotional issues that might have contributed? In their words, yes. Does that mean they should not seek medical advice? No.
Cranial osteopathy (CO) and CST are often used synonymously meaning a system based on gentle manipulation of the skull and sacrum to faciltatet unrestricted movement of the cerebrospinal fluid.
I found this -> http://www.healthandgoodness.com/Therapies/what_is_cranial_osteopathy.php article in which both Sutherland and upledger are mentioned in the context of (CO)
I agree that they are used synonymously which is wrong. The artcile you cited is good for the most part. They do talk about Sutherland and Upledger . What the author should have done when getting to Upledger was mention that he developed Sutherlands work even further. There are a great many quotes that follow in her Upledger section, all without reference.
This one:
“There isn’t any convincing model for cranial osteopathy, even though we know it works. Personally I feel we are working with electromagnetic fields in the body – I often feel heat as I work, and sometimes tingling.”
I find hard to believe came from Dr. Upledger, especially as he spent so much time at Michigan State working on Dr. Sutherland theories. If it was from Dr. Upledger I would love to see the whole article to get the context.
The differences are subtle but they are there.
Here is an article written by Dr. Upledger.
http://www.massagetoday.com/mpacms/mt/article.php?id=10571
Well – that is not the only strange thing he has said. For instance in his book : Upledger JE. CranoSacral Therapy: Touchstone of Natural Healing. Berkeley, Caliifornia: North Atlantic Books, 1999 he describes an incident where he communicated with a 4 months old french childs “inner physician” through the craniosacral system. In his own words:
And through asking yes and no questions to this “inner physisian he deduced that the babys problems was caused by
Another question that arises is if the rytmic movements observed during brain surgery are inexplainable through normal well known physiological mechanisms. This has been looked into by a group of french biophysicists. Their conclusion is, that it is fully explainable through ordinary cardiovascular physiology. Source: http://www.ncbi.nlm.nih.gov/pubmed/2173359?dopt=Abstract
Also this article -> http://faculty.une.edu/com/shartman/sram.pdf discuss some of the problems with the system described by Upledger.
I concur with what David Tomlinson has said about what craniosacral therapy is and what it is like when it is practiced correctly – Safe and Gentle.
Philosophical debate aside as a craniosacral therapist and craniosacral therapist trainer this incident has left me upset. It is just bad all around. It is bad for craniosacral therapy. It is bad for the ‘therapist’ involved.
But the people I can’t get out of my mind are the parents and the baby. I can’t imagine how the parents must be feeling.
My heart goes out to them as do my deepest condolences.
nicely brought back to what is important here
So I wondered when we were going to get here. I’m assuming we’re now done with the reason this all started.
I find it too bad that people don’t take into account decades of practical experience. They focus on a few select quotes that get generated over and over again. Einstein still gets grief for saying that imagination is more important than knowledge.
Why not give context. Dr. Upledger was treating a 4 month old baby who was being called “floppy”. He was very flaccid and had a weak cry an had not progressed much since birth. Then we go through all the stuff you mention. At the end of the treatment the baby began to wiggle around and cry. When in France 5 years later Dr. Upledger was told that the baby had normal development and was now in preschool.
Now, might he have arrived there without treatment. Maybe. Nobody will ever know. Is it at least interesting that the baby began wiggling and crying as Dr. Upledger worked on him? Yes.
People tend to pick out the story and forget the results. If the mother has said she noticed that her pregnancy changed when her husband had been working with the solvents and that her baby had been been born “floppy” make you feel differently? Really what matters here is that the baby is better. They used to drill holes in peoples heads to cure headaches and remove demons. We now know that doesn’t work so well. I would invite you to do some dissection work on a “fresh, unpreserved cadaver” of adults and explain to me why you can find blood pooling in the sutures.
About your articles:
James N. Norton who is part of the article you cited also wrote this:
Failure of Tissue Pressure Model to Predict Cranial Rhythmic Impulse Frequency
J.M. Norton, Ph.D.
Journal of the American Osteopathic Association, Volume 92, No. 10, October 1992
In this work, Dr. Norton investigated the possibility that the cranial rhythmic impulse (craniosacral rhythm) might be the result of some complex interaction between the cardiovascular and respiratory activities. The latter two activities were recorded by skin surface electrodes and pneumograph, respectively.
While the cardiovascular and respiratory activities were being recorded, a therapist practicing CranioSacral Therapy used the knee-switch method described in Norton’s previous work (above) to record the beginning of each flexion phase of the craniosacral system on 20 different subjects. The rate of craniosacral system activity on all subjects was between 6 and 10 cycles per minute.
Norton could find no combination or interaction between the cardiovascular and the respiratory activities that could explain the findings of the craniosacral system examiner. Further, it was observed that when subjects voluntarily held their breath, the craniosacral system activity continued, apparently unaffected.
Dr. Norton concludes that the craniosacral examiner must have indeed perceived and recorded another rhythmical activity besides the cardiovascular and respiratory rhythms.
There’s also this:
Recording of Cranial Rhythmic Impulse
Milicien Tettambel, D.O., et al.
Journal of the American Osteopathic Association
Volume 78, October 1978, Page 149
Dr. Tettambel used force transducers taped one across the frontal bone and one across each of the two mastoid processes of the temporal bones on 30 subjects ranging in age from 16 to 71 years.
She successfully recorded three separate rhythms on all of these subjects. The cardiac pulses and the respiratory rhythms were clearly recorded. A third pulse was also recorded at an average of 8 cycles per minute. She presumed that the third rhythm represented the cranial rhythmic impulse.
I’m not going to try and change your mind, and lord knows you’re not going to change mine. Are there a lot of therapies and therapists out there taking advantage of people when they are at their weakest and most vulnerable? Yes there are. Should they be stopped. I believe so. Is it time for the medical model to move beyond the double blind study? In many cases yes it is.
I need to get going. I don’t want to get into a tit for tat debate here. I’ve done it before and really, I want to spend some time with my kids.
Well – you were the one who found it implausible that Upledger would say:
I think that the claim of having communicated in english with the inner physician of a 4 month old french baby makes it a bit more probable that he could have said as quoted.
It doesn´t have to be a randomised double blind study. But a decent controlled study to eliminate bias from placebo effect and natural history of the condition treated would be nice. For instance could it be possible that the positive effect you and the babys mother observe is a relaxtaion response caused by the gentle touch and calming manner from you?. And is the effect long-lasting?. Thats the sort of questions controlled studys can help answer.
Fair enough.
Sounds like a good idea – Enjoy 🙂
I agree with David. Forceful or hard thrust manipulations are not part of pediatric craniosacral therapy. Please check your sources.
What sources should we check?? The man calls himself a craniosacral therapist, the has a sign by his door on which it says “Craniosacral therapist.” He has a certificate on which it says that he passed the tests for craniosacral therapy. What is there to check?
There ae lots of different therapies out there. Read the article and look at what techniques were being done. Then call any of the big schools of CST..Upledger, Bio Dynamic. Ask them if they teach their students to do manipulative thrusts on anybody. Then make a decision. I can tell you that of all the big schools of CST, who offer some form of certification, there is no manipulations taught.
So if he also had “minister” on his door, would you say that a minister killed an infant?
I think the point is not what the articles or books say what should be done and what shouldn’t. The point is what this man actually did in his capacity as a craniosacral therapist. He was officially registered as a craniosacral therapist, but given what happened to the infant probably not a very good one. The fact that he did a bad job however doesn’t mean that all of a sudden he was no longer a craniosacral therapist.
Um, perhaps chack what OTHER signs and what OTHER traning he may or may not have had?
Perhaps explain here what laws in the Netherlands allow or do not allow someone to call themselves “Craniosacral Therapist” and what the licensure process is? In some countries, such as Canada, there is no legal authority to dispense this title and therefore it is meaningless. Someone who has never touched a human body before can use these words on a door even though most people will interpret these words in a meaningful way.
(I suspect the issue here will turn out to be one of licensure. The fact that he was REGISTERED with private organizations such as Register CranioSacraal therapie Nederland or Nederlandse Cranio-Sacraalvereniging means nothing more than he might have paid a fee to do so. In the USA, the title “CranioSacral Therapist (CST)” is a registered trademark of the Upledger Institute and is only awarded after
severe evaluation of a therapist’s skills. Still, there is no government board certification as there is on a state level for massage therapists or doctors.)
And please, do follow up on your promise to post a full translation of the article by May 8. Until then, no one can truly comment on this tragic event–we are reacting to hearsay.
The fact that you have stayed on point around all of this made me wonder if I had missed something. Here is the google translated version, I don’t speak Dutch after all. The translation also lost some pieces but you get the idea. Sorry about the long link, I don’t know how to shorten them, if it is possible.
http://tinyurl.com/r77rtf
This version varies greatly from the first translated version I read. I wish I could remember who I used. The biggest difference is that this version uses the words “CranioSacral Therapy and CranioSacral Therapist” The first version did not which is why i jumped all over the title of the article. I know understand your point above. I still have issues with certain parts of the article which I will cover.
I will say that if this therapist was doing Manipulations and saying they were CST, by all the standards I am aware of, that is wrong. I still stand by the fact that no CST schools I know of teach Manipulations as part of their training. I do know some Osteopathic schools (European and North American) cover CST. Because of their profession they also teach manipulations.
Should forceful manipulations be done to a baby? In my opinon, No.
I still come back to this, which is their “learning” section;
“There is no scientific evidence for the efficacy and safety of forced manipulation of the spine in children.
Forced manipulation of the spine in an infant can lead to serious complications. ”
I will again say. CST does not involve the forcing of anything, including vertebrae.
I would invite you to read the reaction at the bottom of the page. i think it is very well worded.
Don’t let the actions of one therapist cloud the entire therapy. I understand you want more research into the therapy. I for one would welcome it.
If I’ve missed anything, I’ll add it later. I’m actually enjoying this discussion. I have had so many with people who call themselves skeptics who are really just angry people who seem to have some kind of vendetta against anything they don’t understand.
I look forward to your response.
Re: the What’s The Harm articles:
Neither of these articles are related to CST in the slightest.
Note that Michael Arditti ended up in the hands of the cranial osteopaths due to his own allopathic doctor’s failure at diagnosing the same life-threatening infection the osteopaths missed, instead diagnosing sciatica.
The second article was written by Stephen Barrett, who runs the Quackwatch website out of his basement. The article has so many bias points, it is impossible to start commenting on it. He uses a small event totally unrelated to craniosacral therapy and uses it to put forth his standard rambling agenda against anything non-allopathic: a patient is given advice to discontinue medication, follows that advice, and dies. This has nothing to do with anything other than a poorly trained person giving bad advice.
The point is there are good doctors, and bad doctors. There are also good “toolboxes” and bad “toolboxes”–the frameworks doctors are taught. The cranks are always pointing out the bad ones to discredit larger entities which may or may not be related. The people who benefit from the good ones are happily cured and usually don’t bother to post “I’m cured! I’m cured!” all over the internet. They just go on with their lives.
Registration requires at least a 4-year education in the field at a vocational college (with government accreditation). We are aware of the situation in Canada. The Netherlands is different however, we have compared the rules and conditions in the USA and the Netherlands and they are virtually the same.
I think you might have a valid point there. It seems to be the words “forceful manipulation” that the commenting CST´s feel disqualify the given treatment as genuine CST. But when you think about it you really don´t need any significant force to flex such young babies necks. They dont even have enough strength to keeps their heads upright on their own. One article by an alternative practitioner (CST-therapist??) reports the findings of diverse adverse effects of CST. I dont have access to the full article, but the summary can be found here -> http://www.bodyworkmovementtherapies.com/article/S1360-8592(96)80003-9/abstract
Most of those reported side effects were related to lesions of the central nervous system. He explains most of (but not all) of the side effects as a consequence of treatment performed by “lay-practiotioners”. And they were
could it be spontaneous recovery??
Hi Jli,
I’ve just translated the greater part of the article, so you can read in detail what happened to the baby.
You seem confused about what Craniosacral Therapy involves. There is NEVER flexion of ANY sort (mild or forceful) anywhere on the body, especially the neck or spine, nor is there ever pressure applied of more than 5 grams. Ever. This is why it is evident that the practitioner described in the article was not performing CST. Again, a CST practitioner NEVER attempts to move body parts (i.e. flex).
The 5g pressure is what it takes to lift a small coin (0.20€). You can picture this force by holding the coin on the tip of your finger and holding it. If you push up hard enough to raise the coin, this is more than 5g. This is why, unless the patient has existing intra-cranial pressure issues, CST is harmless.
As well, the fact that newborns cannot hold their neck up on their own is a factor of incomplete muscular development, thus having nothing to do with their ability to withstand flexion. You don’t depend on muscle resistance to determine the amount of flexion you apply.
I don’t know that I’m confused. Couldn’t it be that the craniosacral therapist was confused?
Thank you for the translation in progress.
>Then she was turned to her right side and a
>deep bending of the vertebral column was
>applied at which the chin touched the chest, as
>shown in figure 1
This is not CST. Period.
This has the look and feel of chiropractic.
Sounds like she suffocated. Babies are very fragile. Holding them too tight can also produce this. It is horrible. The person who did this had no idea what he was doing. To try to blame whatever therapy he thought he was trying to perform is ludicrous.
It happens too frequently in hospitals that a nurse misreads a doctor’s scrawled dosage on a patient’s chart and administers the wrong amount of medication. When a patient dies because of this, we do not blame the practise of nursing in general, but try to find out what happened in the particular case. If the individual nurse is liable, action is taken. The story ends there. Why should this be any different?
My reply was to jli, who does seem confused.
Which means you are also confused, thinking that my reply was directed to you. 😉
I don’t know if the person you are calling a “craniosacral therapist” was “confused”.
I do know that anyone in the healthcare profession (doctors, chiropractors, CSTs) should know better than to do what was described in the article, or should not be allowed to practise.
I also know that what was described qualifies as “negligent homicide” in my book.
What we are all trying to get across to you here is that the title of your blog “Infant Dies after Craniosacral Therapy” is fallacious and inflammatory.
The point is the infant is dead. Let’s try:
“Infant Dies after Unqualified Idiot Either Suffocates Her or Damages her Spinal Cord”
Translation is completed.
Quote:
“There is NEVER flexion of ANY sort (mild or forceful) anywhere on the body, especially the neck or spine, nor is there ever pressure applied of more than 5 grams. Ever.”
Hmmm – AKA homeopathic manipulation??
Quote:
“…anyone in the healthcare profession (doctors, chiropractors, CSTs)…”
FYI – Two of these aren’t professional healthcare.
I absolutely agree. Doctors and chiropractors. 🙂 The former being a glorified plumber.
Very snappy. Obviously you have homeopathic openmindedness and understanding of the human body. 😉
Open to actual medicine, not health fraud.
My point exactly.
What would we do when a conventional doctor screwed up? Would we stop calling him a doctor all of sudden, just because it makes the other doctors feel uncomfortable?
This man was a craniosacral therapist. To me there seems to be something wrong with the system and I think that is what we should be looking at. Changing the title of the post won’t solve any problem.
Yes. If a conventional doctor screwed up by performing an operation that was not sanctioned by the College of Surgeons and it resulted in a death, we would make him stand trial for negligent homicide, strip him of his title of doctor (i.e. retract his license to practice medicine) and not blame the ENTIRE medical profession.
He might henceforth claim he is still a doctor, but the community of his peers, the College of Surgeons, has rejected him and pronounced that he is not a doctor any longer for having done what he has done.
There is little wrong with the system. Anyone can qualify with promises and not follow through, no matter the profession. A bad man does a bad thing and is punished. It happens every day, regardless of systems of belief.
That addresses the issue of incompetence. The problem with the title of the post is an issue of bad journalism, and this is entirely your problem, not society’s. I suggest you take responsibility for it, since this is your blog, instead of hiding behing unending sophistry.
You are not doing anything here other than engaging in poor, irresponsible journalism with an axe to grind. In the US, we call it FOX News.
It is uninteresting, insulting to human intelligence, and dangerous to human life.
Since they also appear in the title of the orginial article, I have just added inverted commas.
I’m not hiding behind anything and I have translated the article ad verbum, albeit in decent English instead of Google non-speak.
I am curious which school it is that has a 4 year educational process for CST. Could you provide a link for me please. I’d love to know more about it.
Thanks you for providing the translation. It is much better than my nonsensical translation via Google.
I agree with Michael that there is journalistic integrity/responsibility that comes with hosting a public forum/blog.
Correct me if I am wrong but there appears to be a bias against CST for various reasons. That bias seems to have influenced the posting. Instead of posting about the Therapist, you chose to align the entire therapy with one bad act. That is wrong.
I´m not eduducated in CST, so I have the right to be :-). Anyway the situation is that a therapist claims he treats people with CST, and you claim that he doesn´t (at least not in the case discussed here). So it is your words against his. Why should we believe you more than him?
Don’t believe anybody. Not even yourself. Do research on the therapy. Call the schools, gather information and then submit a well researched, thought out and written article.
You mean only the schools you aknowledge of course – Not the one that the therapist in question attended. I think we will have to settle with your words against his.
I don’t know if I would call it bias. It’s just that the efficacy of craniosacral therapy is being disputed.
When did I do that?
If what you say is true and this is not craniosacral therapy at all, then the parents were severely deceived. But that’s not all. If it is possible that a registered therapist applies a treatment that is completely out of line with his professional standards, then there is a problem in the Netherlands regarding the training of and evaluation of craniosacral therapists. That problem should be fixed in my opinion.
wow. Nice. I mean every school. How do you generally do your research? Only call those people that would support your writing? Why wouldn’t you call the school in question? That’s daft.
Also,
If you truly are wanting to “settle this” with a our words against his, then you do not understand researching an article
There are two “schools” in the Netherlands that are acknowledged by the Dutch government and of which treatments are funded by most health insurance companies: the John Upledger Institute in the Netherlands and the polytechnics (higher vocational colleges) for Health Education that also teach cst. Next to these, there is a number of other facilities where you can also study craniosacral therapy.
I don’t think we need to call all the schools to ask what exactly they are teaching and compare this to I don’t know what really. When someone graduated as a cs therapist clients should be able to expect the therapist to be knowledgeable and professional.
Exactly 🙂
I think you have been fair to the visiting CS-therapists. They have been allowed to post any comments they like – without any censorship at all. Surely their beliefs have been questioned by some posters (including myself). But is that so terrible? Personally I welcome them to express their views – even if I disagree. And I´m willing to accept that the therapy given is not the kind of CST they would have given.
Wonder what happened to:
You don’t need to call _all_ the schools. My point was in reaction to Jli saying to only call those we acknowledge.
Why do you want to compare schools? I would think the question to be asked would be along the lines of…”do you teach forced manipulations as part of your CST Training” or some such question.
Do you often have to censor threads?
I am more than willing to have my beliefs and the therapy questioned. I tell people to question everything until they are convinced for themselves.
I still firmly believe that CST should be studied. My wife and I are beginning to work on just that. If you have any input, please let me know.
I think we’re getting to the end of this. I’m sure we could keep going round and round on some of the issues..who knows, we may ;o)
what happened to not wanting to get into tit for tat. I didn’t with where you were going jli. beatis was staying on topic..and I had just spent a load of time with mu kids..lol.
I appreciate the forum for this discussion. A majority of the conversations I have had surrounding CST, I leave because the other people are not educated about their topic. They are only spouting off others peoples words with nothing original added by themselves. It gets very frustrating.
I’m off to study wind with my wife and kids.
Then I misunderstood your meaning.
No, we don’t. We censor comments that are used for pitching, that’s all. However, I’ve been censored myself quite often: I’ve posted comments on a number of blogs on alternative medicine and most of them never made it through moderation.
That sounds interesting. It would be nice if you will let us know about it.
Have fun! 🙂
jli, you have the right to be as “un-eduducated” as you want. 😉 However if you are going to discuss something in a public forum, you need a modicum of good information about something to make statements about it, otherwise you just look like a fool who is pulling thinks out of his bodily extremities…
Again, I bring you back to the example of rogue MDs, who have their licenses yanked and get sent to jail for doing things the Medical Boards have decided are not Medicine. This happens frequently, because there are idiots in every profession. Is this a problem that needs to be addressed according to you?
Please describe in detail the licensure process that a graduate of one of the CST schools in the Netherlands goes though. Who is the governing body? What exams do they administer? What degree and title to they bestow?
Or, is it more like a plumber? Anyone can call themselves a plumber and do carpentry on the side.
And finally, if it’s my words against “his”, does this person have a name? Have you actually asked HIM if he thought what he was doing to that baby was CST? And who he studied with? What diploma he has? What certification? What license? Other than a sign on the door? If not this is hearsay, and you are behaving VERY irresponsibly.
Jli is not Dutch, so he can’t go into the situation in the Netherlands.
Of course it is.
I have explained about this in an earlier comment to David Tomlinson.
This person does have a name, but I will not disclose it here. Of course he thought what he was doing was CST, he advertised himself as a CS therapist.
The report tells in detail what happened to this baby during and after her treatment by a so-called “craniosacral therapist.” It was written by the physicians who were involved with the baby after she arrived in the hospital. Nowhere does it say that the CST was the cause of the infant’s decease. All parties involved have given permission for the publication of this report, so I really don’t see any element of hearsay here.
Of course – and it is beeing addressed all the time. But this thread is about someone claiming to use CST, and when doing so things went terribly wrong. You seem to think that this should be an exception of what wrong doings can be discussed in public. You didn´t accept the examples on “whats the harm” as examples of wrong doings through CST – okay then don´t. The examples were brought forward for comments. And commented they were. You never addressed the article written by an alternative practitioner describing side effects of CST (when performed badly). That is your right of course. I´m just trying to understand what went wrong in the context of CST. I see no reason to mistrust the blog owners when they bring this case report forward – but apparantly you do. That is your problem – not mine.
I’m baaaackk lol
“nowhere does it say that the CST was the cause of the infant’s decease.”
except the title of the posting. If it doesn’t say it anywhere in the article. Whose idea was it to publish under that title? Where did you find the article..who published initially?
I look forward to the Reaction being published.
and anybody with higher brain powers is going to link them. This goes to responsibility in reporting.
There’s a difference between “Gerry dies after golf”, and “infant dies after CranioSacral Therapy”.
A more suitable title might be..Infant dies after therapist practices outside scope of practice.” Could you then talk about CST? Of course.
I hadn’t looked beyond the ref’s..my bad. Thanks for pointing it out oh newcomer.
Translation is completed. It’s at the bottom of the post.
Knock off the personal insults already, David.
Stop your insults too, Michael.
How is suggesting that anybody capable of critical thought could see thedifference a personal insult?
There are certainly more people than on this blog reading the article. I was meaning the bigger picture world.
Sorry, but I am not aware of having insulted you. Would you refresh my memory, please?
Not in any meaningful way and certainly not answering the questions I asked. Are you avoiding them?
You talk about “registration”. Again, will anyone paying the fee and waiving a diploma be given the title “Craniosacral Therapist”?
Who has registered the trademark “Craniosacral Therapist” in the Netherlands? Which LAW has decreed that a particular organisation can register or certify this profession? If either of the above two things have not been done, then, legally, there are NO craniosacral therapists in the Netherlands. Just people who decide to call themselves this, and this is a problem.
What are the names of the ACCREDITED colleges you mention that teach a 4-year program in CST?
Are there exams? Peer evaluations as there are at Upledger Institute USA to receive the certified moniker “CST”?
It sounds from what you have said so far (very little) that it is easy to earn the “right” to call yourself CST in the Netherlands and that pretty much anyone can do this, even though they may not be qualified.
This is a logical fallacy. You are attributing intent to someone you have not spoken to personally. Therefore hearsay. I know many MDs who perform acupuncture and homeopathy. The sign on the door says “MD”. But the MD KNOWS he is doing acupuncture and would not claim he is practising medicine at that very moment. I’m sure you are smart enough to see where I am going with this. If a lung is punctured in the process of this MD giving acupuncture are you going to write an article entitled “Child dies after receiving medical procedure”? No. you are going to belittle the MD for having poor judgement and bad skills at _acupuncture_, not medicine.
You should either come out and say that “all craniosacral therapy is bad” or stop trying to _imply_ that craniosacral therapy was actually practised and therefore is connected with the death of this infant.
We are repeating ourselves at this point. I think there is a language communication problem.
Which is the red herring.
In this particular case, CST was obviously not used (according to the experts in CST), so discussing the merits and problems with CST is irrelevant and unnecessary.
In the current legal system, everyone is allowed one “bad”, whether it is a mistake or a purposeful act. You cannot catch a criminal before he/she performs the crime.
In allopathic medicine, a medical license to practise is automatically renewed UNLESS there is a complaint or disciplinary action that justifies not renewing. Again, the first “bad” is free. No way of preventing it. So I’m not sure how you would have prevented this death in particular in ANY healthcare profession.
If anything, the PARENTS need to take a good look at their responsibility here. Did they fully understand the procedure they were signing their baby up for? Did they get sufficient recommendations? Know that this practitioner had treated other babies with the same symptoms as their own child? That he had no other complaints or legal action against him pending? There are so many unknowns here–so many other way to approach the “blame-game”.
Translation please?
No.
What does “QFT@JJ” mean?
In English: “translation please”
QFT means: quoted for truth.
See: http://www.urbandictionary.com/define.php?term=QFT
JJ is JennyJo.
@ Michael Ross:
Re your comment of 3:57 am
The John Upledger Institute Nederland organizes trainings for CS therapists. They work closely together with the American John Upledger Institute. When you have had training with this Institute, your treatments are payed for most Dutch Health Insurers (with a maximum).
http://www.upledger.nl/
You’ll have to trust me for giving the correct information, I’m not going to translate the complete web site.
Then we have the public colleges (public as in: not private and funded for the greater part by the government) for higher education (known in the UK as polytechnics). They have courses teaching fysiotherapy, manual therapy, other kinds of massage and also cst. These courses last 3 years, followed by 1 year for a master should the student want to do this. When you have graduated the 3-year course, your treatments are automatically payed for by most health insurers (with a maximum).
Then there are all kinds of private institutions, both in the Netherlands and abroad, where you can also learn to be a cs therapist. Some of these are acknowledged by the John Upledger Institute and are then payed for by most Dutch Health Insurers (again: with a maximum).
When you want to be acknowledged by the John Upledger Institute, you have to pay a fee. There are 2 professional organizations of cs therapists apart from the JUI; membership is not mandatory and is not cheap, therefore not all cs therapists are registered. Some of those have received excellent training, others have not. Not being a member of a professional organization does not automatically imply that someone is not a good cs therapist.
Re: your comment of 4:14 am
This is where we disagree. When someone has a certificate stating that he is a professional cs therapist, the parents should be able to expect the therapist to be knowledgeable and professional. It is the responsibility of the sector to ensure this. When a child dies after treatment by a conventional MD, we don’t go and blame the parents for not having selected a better doctor. Then why should we have to do this when a problem arises after treatment by a cs therapist?
That the efficacy of CST is being disputed is no secret and I don’t see what’s wrong with it. There is a lot of money involved, a large part of the health costs, including those for CST, are being funded via taxes in my country, as in quite a number of other countries in Europe as well, so I don’t see why we shouldn’t discuss efficacy. There are procedures in conventional medicine as well that are being disputed. I don’t know how it is in your country, but in mine certain spinal operations are no longer performed and/or no longer refunded as a standard by health insurers because the usefulness is unclear, which is acknowledged by the medical profession as well.
Are you sure this is a logical fallacy? 🙂
When a person:
Says he is a cst
Offers and applies “craniosacral” treatments
Charges money for these treatments
Makes a living as a cst
Has a diploma saying he is a cst
On what basis then am I to question his being a cst and his intention to act as one? I don’t see the fallacy.
An MD is always an MD, he is also an MD when he is doing acupuncture. He cannot ever not be an MD, unless he has his licence revoked. He could not claim not to practise medicine when he is giving acupuncture. People should be able to trust him as an MD at all times, no matter what treatment he is giving.
Yes we have established that many comments ago thanks to the visiting experts in CST.
Now – as a layperson, how is one to know that a practitioner with a CST-diploma who claims he is giving CST is not giving CST?? One could of course ask another CST-pratitioner – but that is not how things work. Don´t you agree that it gets even more difficult for a layperson to know what is real CST and what is “fake-CST” when as one of the experts put it:
Damn, the Quack-o-meter(tm) babble translator overloaded and burned out…it now needs both the wall-of-words and bullshit bedazzler modules replaced.
That is an excellent point and needs to be looked at. What happens with many modalities is that people take a course and decide that they can start teaching on their own. This lead to many unqualified practitioners in a great many fields. CST is included in that.
It is completely reasonable to think that if you are going to a person with a diploma, calling themselves CS Therapist that they have a certain level of skill/knowledge.
I know I tell people who are looking for a therapist to call many different people and talk to them. Still they could make a decision and the results could be very bad.
There need to be greater controls.
I need to run. I wanted to start a reply to this. I’m hoping to get to more of it later.
Sorry for the partial posting.
My point exactly.
Thank you!
Wow, that’s a really mature comment…. I’m sure glad you have decided to make a meaningful contribution to this discussion, which is actually getting somewhere, despite you.
BTW WordPress has decided to stop threading this topic and is posting all new comments at the end. It’s difficult to tell who’s replying to what. Is there any way to fix this?
Well there’s something we agree on..and have for a while now :o)
Every year you hear of people going to jail for practicing some form of medicine or therapy without a license. Can we stop people from setting up their own little practice with little training. Unfortunately not with great results.
In the case of someone who is fully qualified (whatever that means) and granted a diploma by a school, can we stop them? We can take away their license and diploma, throw them in jail if warranted. Can they then move on and set up shop somewhere else? If they want to.
I honestly think we’re in agreement on a great number of points here. Greater controls and proof of efficacy being the main ones.
I have taught in a bunch of different countries and in almost every one I have heard stories of people taking at least the first level, of at least 6 in a linear direction and beginning to teach the work as their own. Complete with reproductions of the study guides we use.
That is an unfortunate fact of people having no ethics/morals/conscious/regard for the safety or well being of others. For those people, who have not even begun the certification process, taking away their ability to do the work will do nothing. They will do it anyway.
Has the court case happened? If so what was the result? I would be very interested to hear what the courts have to say and read a copy of the court transcript before I comment too much further.
I know it must be hard to act as you all are doing..exposing frauds as you see them. It takes a certain amount of determination and possibly even anger to drive it. As you have said you are censored on various blogs because of your posts. Again that is probably very frustrating.
Without Critical thought science and medicine would not be where they are. I know Dr. Upledger has one of the biggest left brains I have ever met. Please keep people on their toes but can I ask you to remain open to all the evidence that is there on a case by case basis, that shows that the therapy does have some efficacy to it.
There’s a maximum of replies in every thread. With every reply the layout becomes narrower, which makes the replies more difficult to read the more there are. There’s no perfect solution I’m afraid.
What you can do is first of all indicate who you are replying to, for example: @ Beatis, and then copy the url of the comment you are replying to in your own comment. Like so: Submitted on 2009/05/17 at 9:14pm
I’ll try to keep you posted.
@Michael Ross
“Wow, that’s a really mature comment…. I’m sure glad you have decided to make a meaningful contribution to this discussion, which is actually getting somewhere, despite you.”
Oh you haven’t seen anything yet michael… a few of us have noted the childish comments and lack of meaningful contribution displayed by evenarsenic…
@evenarsenicisnatural
i find this hilarious “evenarsenicisnatural // May 16, 2009 at 11:54 pm | Reply
Stop your insults too, Michael.”… followed by evenarsenicisnatural // May 17, 2009 at 2:18 pm | Reply
Damn, the Quack-o-meter(tm) babble translator overloaded and burned out…it now needs both the wall-of-words and bullshit bedazzler modules replaced.
is that not insulting???
To beatis:
There is a severe problem with WordPress. I got an email notification with your post “Why the double posting?” but it does not show up for me here. Same with both posts by “anon”, which is likely why they double posted, if they could not see their own post…
Anon –
It’s only insulting because it’s true.
So personal attacks and preaching health fraud are noble, eh?
I’m sorry about the glitches, but there’s nothing I can do about it.
Yes
There’s no need for me to speak to him personally. He advertises himself as a SCT and gives treatments labelled “craniosacral therapy.” That should be enough for anyone.
What I mean is that people will trust an MD in his capacity as an MD, no matter what treatments he is giving. When he harms patients while treating them with acupuncture and his expertise as an MD is questioned because of this – for example when a judge thinks his medical licence should be revoked, he can’t say: o, but while I was doing the acupuncture I was not an MD but an acupuncturist so my medical license has nothing to do with it.
So when John Upledger, MD, practises CST, as he has done for the past 30+ years, he is practising medicine? This is good news for you and for all recipients of CST!
No, I mean an MD is always an MD. And as far as I’m concerned, acupuncture is always quackery.
Unless you are posing as a journalist, which is what is implied by publishing this blog.
Yes, again, if you are performing poor journalism and not actually asking intelligent questions but are scrambling to just make a point and push your not-so-well-defined agenda.
Perhaps this is what you would _like_ to say. But your fallacious arguments lead you elsewhere….
Wow. So much for understanding global medicine, in which acupuncture has been practised in Asian countries longer than MDs have been –literally– bleeding patients and putting leeches and suction bulbs on their backs.
You are of course entitled to your opinion, but you should realize that statements such as that make you appear incredibly short-sighted and narrow-minded.
Personally, I don’t like tofu.
Well, we’ll just have to agree to disagree then.
@ evenarsenicisnatural
“So personal attacks and preaching health fraud are noble, eh?”
I don’t know, are they? you seem to be the one full of double standards…
Awww, you dropped your binkie.
@evenarsenicisnatural
“Awww, you dropped your binkie.”
I get the feeling you don’t like answering questions? is that right?
Anyone other than me get the feeling that even and anon are just parts of the same person’s schizophrenic brain? They sure like talking at each other… 😉
Not really…
Seems like Michael Ross is the only one who gets that feeling.
Was just sent this link. I don’t think this has been posted. What I find interesting are these two paragraphs quoted in partial.
“The Nederlandse Cranio Sacraal Vereniging (Dutch CranioSacral Association) does not recognise this manipulation….
The therapist is not known at the professional association. The spokeswoman says that this could indicate that the practitioner isn’t certified.”
I’m curious where this person received their qualification to practice from.
David
http://www.digitaljournal.com/article/272986#tab=comments&sc=0&contribute=&local=
Thanks! I read it in the Dutch news but didn’t have time yet to translate it.
It is very simple, really. You do a large study, get the results published in a respected journal. Others will be motived to do the same, and if the results overall are more positive than the placebo effect, medicine will have one more therapy at its disposal. If not, then not.
To the best of my knowledge, such evidence does not exist. As long as it doesn’t, anyone is rightfully highly suspicious of CST, and well-advised to stay away from it.
“Is your comment directed to me?”
Mine wasn’t. It was meant as a reaction to the idea that an MD practising some type of quackery is not an MD at that very moment.
I also saw this:
“Is it time for the medical model to move beyond the double blind study? In many cases yes it is.”
That’s quackstuff. The double blind study is the best we have so far. When an alternologist says that it isn’t capable of detecting the results of her/his specific type of alternology, he/she is simply saying that his/her alternology does not work. Either there are results or there aren’t.
@ Michael Ross, https://anaximperator.wordpress.com/2009/05/07/infant-dies-after-craniosacral-therapy/#comment-1081
I see. And is that also what you would say about Merck and Vioxx, or would you simply say what most alternologists say about what they so elegantly call “Big Pharma”?
Pingback: Cranio-Sacrale therapie en andere W.C. eenden. « Cryptocheilus Weblog
There have been new reactions to this article by the professional society of cs therapists and the MD’s who treated the infant. Translations will be added to the post in about 24 hours.
Ok,
so you tell me how to double blind a hands on manual therapy.
1. The client would not be able to know they were getting the therapy..easy enough
2. The therapist would not be able to know whether they were doing the therapy or not.
If what you say is true and such a trial is really impossible, then you are not entitled to claim any effects of CST.
But perhaps craniosacral therapists could start with generating evidence for the underlying assumptions of CST.
Btw, I found this on the internet: http://www.chspr.ubc.ca/files/publications/1999/bco99-01J_cranio.pdf
And this: http://www.spiked-online.com/Articles/00000002D402.htm
Let´s see if we can come up with some sort of idea on how to blind the procedure. Your point 1. seems not to be a problem. I would prefer some kind of blindfolding of the patients (I know you called them clients, but please – go along with me) to ensure that they don´t pick up on the therapists’ signals of expectation.
With regard to the therapist not knowing whether they gave the therapy or not (your point 2.), you could simply let somebody else evaluate the effect of the given treatment. You would then have a patient not knowing if he was given CST. And you would have an assessor not knowing either. All you have to do now is to define the group to be randomized and the parameters to assess the effect. It is not more complicated than that. 🙂
hey,
I don’t even know if the client has to be blindfolded. I think just lying there with eyes closed..or open would be fine.
As for the effect of the treatment…Range of motion could be used…a subjective pain scale could be used. I know the Physical therapy studies use a subjective 1 -10 scale in some studies. ” I came in with pain..I’m leaving with none”
You could piggyback on other studies. Take a P.T study for back pain (for example). Let’s say they treated 20 people and had 20 people as a control who had no treatment. You could take 20 people and treat them with CST an combine the results.
Why not outcome based? I treat 20 people with back pain 12 get notice great improvement, 5 moderate and 3 notice no change. It gets rid of the need for a control.
Over the past 16 years and the thousands of people I have worked with, I can easily claim success of many things. I have treated hundreds of babies with colic…90 some odd percent have had no colic afterward. The same goes with breast feeding issues and reflux. In adults I have worked with PTSD, Chronic Pain, TMJ Issues, headaches..I could keep going. Have they all miraculously become better? Nope. Have a huge percentage of them noticed a dramatic difference in their pain/condition? Yes. Otherwise I would not continue in the line of work I am in. Do I see changes n people every single day. Nope, I don’t wok every day ;o)
There was a time when I used to get so worked up talking with people in threads such as this. I would think “how can they be so closed minded..blah blah blah” I’m over that. Honestly, and I mean this in the most respectful way possible. It doesn’t matter to me whether you believe in CST and/or the efficacy of it. I know it works. I’ve treated people all through North America, Europe and Asia. They’ve all noticed change. Change that can be documented. Which I have not done because it doesn’t occur to me at the time. I think of it after when they comment..”hey my pain is way better/gone/different.”
I’m open to doing a study or 2 or three. At some point when the right time arrives for me to do it.
I’m wondering on your (your being anybody of the skeptical side) side, have you tried CST..more than once? I mean giving it a course of treatment..say 5 or 6 treatments (or whatever you wish to call them). I’d be curious to know what your experience was.
Gee, my wallet is so much lighter, but the symptoms returned shortly after leaving the office…must be from all that ‘conventional’ treatment received in the past. I just have to keep returning ’cause he says so, and need to keep thinking happy thoughts.
David’s quackademic scorecard:
Wall-Of-Words – check
Testimonials – check
Must repeatedly return – check
Thousands of suckers, err, customers – check
Works on everything – check
Accusations of closed-mindedness – check
Lack of documentation – check
Who needs facts, just believe – check
Ad nauseum – yeah, ’tis sickening…
see also http://scienceblogs.com/whitecoatunderground/2008/01/quack_miranda_warning.php
it’s for quack products, but also applies to quack treatments
Wow, “even”, that arsenic really has turned you into a complete ass.
Even’s ass scorecard:
Heavy sarcasm – check
Not addressing a word of what anyone says here – check
Flippant – check
Use of buzz words – check
Nothing better to do than hate – check
Ad hominem after ad hominem – check
Pithy but meaningless userid – check
Thinks he’s the thought police -check
Likes to see name in print, even on a blog no one reads – check
Anger due to personal bad experience or friend’s bad experience, or mother’s suicide – check
you’re right. 16 years of practice is because everybody’s symptoms come back once they leave. It’s amazing how over 16 years I’ve had 24,000 single patients. Not one returning person. None who have referred anybody. Amazing really.
I also wonder about the people who have never had conventional therapy for their problem, come in, get better. Maybe it’s a homeopathic effect from all the regular PT out there..just filtering through.
Also, I never tell people to come. Why would I do that? It would then be about me as a therapist and my ego telling someone what they need. People come back on their own. Must be why they refer people as well. Maybe that’s why I have ER docs referring to me as well.
Thanks for continuing to address points in such a well thought out and insightful manner.
David,
What is your point? The subject is how to provide scientific evidence for the efficacy of CST. I don’t see any of that in your comment.
This does not get rid of the control at all. Also, 20 subjects is nowhere near enough. With the number of clients you have it would be easy to have groups that are sufficiently large.
I would like to suggest you read a book on how to conduct a good scientific trial to measure the effect of CAM-therapies. A very good one is Snake Oil Science, by R. Barker Bausell. Don’t be fooled by the book’s title, Barker Bausell is a biostatistician, has researched CAM rigorously for years and is an expert on the subject.
Here is some information on the author and the book:
http://www.sciencebasedmedicine.org/?p=4
http://www.skepdic.com/refuge/bausell.html
http://nursing.umaryland.edu/faculty/osah/bausell.htm
Okay – The important thing is that the only contact the patient has with the therapist is the actual hands on treatment (CST or placebo). No conversation and no eye contact.
Because this would only say something about whether people felt better because they visited you – not if it was the CST that did it.
The comments to this article by a number of CST organizations in the Netherlands, Belgium and Germany have been added to the post, as well as the reply of the MD’s of the University Hospital St Radboud, who treated the infant.
That should be enough I think for everyone to get a balanced view of all available facts and opinions.
Sorry beatis, it’s not. I guess…
Thousand of patients treated by single therapists and not one shred of even flimsy evidence noted in 100+ comment that is in favor of CST. (besides, ofcourse, the usual ‘case reports’)
Ofcourse, evidence in favor of CST is not the major topic in this post, but I find the above mentioned very ‘interesting’, even when tossing aside this very awfull incident (or is it? Is there any serious information on the safety of CST, apart from therapists claiming only succes and no failure on a blog (which no-one apparently reads…)
Yes I know there is evidence that claims otherwise, (like the article on which this post is based), but just give the evidence and we’ll all be fine. With thousand and thousands of treated subject there must be something that is worth a link in the next 100 comments…
We accept side effects because a treatment has a proven effect. That doesn’t mean we accept any side effects; there has to be a profit in the treatment in terms of cure or considerable improvement; there has to be an acceptable balance between what the treatment does – the gain – and what the side effects do – the pain. I haven’t been able to find out what the gain of CST is. But when there is not one single shred of evidence for the efficacy of a treatment, we shouldn’t have to put up with any side effects at all, not even if they are extremely rare or very light.
Couldn’t agree more.
In this case risk awareness seems to be making people head the opposite direction when comparing to, say flushots. Strange. Not one shred of evidence saying: yes this works, but with more than an occasional fatality, but still people are letting their babies getting bent by therapists that don’t seem to be really aware of what they’re doing. (since there is no evidence, either pro or con) Why?
That’s why I have termed this behaviour “paralogical”. These people are perfectly logical: they simply follow the route of least evidence.
beatis – at what you were saying above: that the guy was a ct-therapist full stop – a reason to incriminate the whole branch. i can give you many examples of mainstream doctors from big hospitals who are currently butchering people. with license and all. that doesn’t mean that all drs. are bad. in aristotelian logic what you say is: “one taxi is yellow therefore all taxis are yellow”. i understand that you’re against everything except what we call “conventional” but keep your logic sane.
No it is not. The underlying theory to CST has no plausability whatsoever, therefore the CST for infants is intrinsically dangerous. And useless as well fot that matter.
I am a CST practicioner. Craniosacral Therapy is totally safe, and very good for infants.
Just to put emphasis on what others have already said, CST is very gentle. You don NOT manipulate or bend with force.
Do you have any evidence for this? Since infants are very fragile, especially their heads and necks, I would be afraid of any manipulation.
Can’t believe I’m wading back in here. I thought I would drop by and see if anything had been posted about the court case…any word yet?
Jennyjo..your last few words “I would be afraid of any manipulation.” I agree completely. In no way should a baby have their vertebrae manipulated.
CranioSacral Therapy teaches no manipulations at all. There are are different practitioners who do manipulations..chiropractors, some P.T.’s but that comes with specific training. Nowhere in CST do we teach to use that kind of force.
The court proceedings haven’t been ended yet as far as we know.
I read this today & find it worrying: Chiropractic Association promoting neck manipulation on infants, http://bit.ly/2g2zun. Doesn’t this child need a proper doctor to begin with??
I wonder what the evidence is for the usefulness of this kind of neck manipulation on infants. Or for any other kind of neck manipulation on infants for that matter.
I realise I’m late to the “party”, but I had to come.
“Despite the fact that the authors have been very careful in their search for an explanation for the cause of death of the deceased infant, they do not succeed in establishing the likelihood of a causal relationship between this death and the therapy that was performed.”
This alone is enough to show that the “Manual Therapists” involved in writing this letter are despicable. Who are they kidding?
The CranioSacral Team’s letter is equally despicable. Despite saying that they have nothing to do with this person (as all the CSTs are saying on this thread), they still deny the relationship between the serious abuse of a small baby and her immediately pursuant unconsciousness and death.
“In the article a causal relation is assumed between spinal manipulation and/or forced deep bending of the neck and the occurence of the symptoms.”
Again, who are they kidding? If this person was practicing purely outside any rules of their profession, why do they need to deny that this rogue CST has killed this small child? One explanation is that both groups feel connected to this so-called therapist and so are trying to deny what isn’t exactly rocket science.
For FSM’s sake. This baby was bent and twisted and subsequently died. If you get hit by a car and die in the road, do you think any one’s going to consider the car driver’s argument that really you just had a heart attack when your heart appears totally normal in the autopsy?
Responding to someone’s comment about “real” CST treating “excessive crying” in infants. You know what else treats “excessive crying”? Caring carefully for their needs and waiting until they grow up into beings that can express their feelings in words.
If you are treating “excessive crying” you are treating babyhood-with-worried-parents. You are subjecting the baby to unnecessary therapy, no matter how gentle it is. You are stressing the parents financially; you are preying on their worries.
If you need some tips to help you deal with crying children to pass on (for free, of course) to your clients suffering from the deadly babyhood-with-worried-parents syndrome, I can give you some ideas.
@ Esti,
There you have hit the nail on the head.
Cranial massage for babies is still actively advertised by craniosacral therapists although there is not a shred of evidence for either the plausability of the underlying theory (“the pulsating of various bodily structures in a symmetrical, balanced and rhythmic motion – the cranial rhythm – which also reflects out through the fascia to all parts of the body”) or the efficacy of the treatment.
Pingback: Zembla over osteopaten, chiropractoren en craniosacraal therapeuten « Cryptocheilus Weblog
Pingback: Infant Dies After Craniosacral Therapy: Therapist Gets Off Scot-Free « Anaximperator blog
Esti —I agree totally with your comments. I am a UK Physiotherapist.
This tragic case and some of the subsequent replies leave me scratching my head as to the stupidity of not only the actions but belief systems of the practitioners concerned.As you say in our culture the problems of babyhood and worried parents is a natural market place for those offering ‘treatments’.
Many of the issues you touch on are cultural —working parents, often with no contact with wider family supportive networks to ease the burden and calm troubled children . It is not a medical or therapy issue in the vast majority of cases.
I have a deep interest in the effects of touch , understanding communication through skin contact through efferent channels affecting autonomic processes for example. All this can be explained through biology and modern neuroscience. Unfortunately, I feel manual therapists are often hampered by a reliance on biomechancial principles for explaining treatments or ‘vitalistic’ theories –neither of which are probably that helpful in explaining some of the( often) positive effects when light touch between two individuals occur.
As this case tragically illustrates –faulty thinking no matter how well intentioned can cause severe consequences. Why people manipulate anyones neck at any age is beyond me.
Ah, This is awesome! Dispells some misnomers I’ve seen
Pingback: Worrying: Wordpress shut down a Blog of a Student Critizing the Naturopath Christopher Maloney « Laika’s MedLibLog
does anyone know the current status of this situation?
I practice CST and I’m certified by the Upledger Institute. I take personal responsiblity for my own work regardless of who I am “supervised” by. CST is NEVER forceful.
I treat lots and lots and lots of babies. Parents are not so concerned about the lack of scientific evidence when THEY notice changes in their babies.
Hey Michelle:
No matter how many classes you’ve taken or certifications you may have overpaid for (oh riiiight – ‘earned’), you’re still peddling dangerous, worthless garbage to unsuspecting marks.
Whatever he called himself, or whatever paper was hanging on his wall, the therapist was not properly practicing cranial sacral therapy, which has no forceful manipulations. Further a therapist who persisted with an infant distressed into crying shouldn’t have his hands on anyone.
This is simply a case of malpractice. It should be no more an indictment of CST than the thousands of people damaged and even killed by mainstream medical malpractice or carelessness is a case against all of mainstream medicine or MDs. There is no branch of medical science where certified practitioners haven’t harmed people.
In many of your articles, it is the science or protocol that you rightly question. In those cases, even a perfect practitioner can do harm. But here, you making an argument that would be like dismissing all heart surgery because a few surgeons botched the work. The harm here was done by ineptitude, and would not have been done by a skilled practitioner. What’s needed is not blanket condemnation of methods that have proven very helpful when done properly, but pressure for malpractice oversight and penalties in “alternative” medicine.
You seem to forget that there is no evidence whatsoever for the efficacy of craniosacral therapy as a treatment, nor for the plausibility of the underlying theory. This means that craniosacral therapy as a whole is complete bollocks. Therefore, any comparison with life saving mainstream treatments like heart surgery is stupid beyond description.
You cannot blame any therapy for the damages caused by awful practitioners.We have thousands of examples of conventional doctors’s horribly going wrong because of gross mistakes or plain lack of expertise, and then we blame the bad practitioner not the medicine at large. You are obviously NOT honest in your approach.The supposed cranio-sacral therapist is a demented case, you cannot apply that kind of therapy to a baby, you do not need even to be a doctor to perceive this.
We do not “blame” craniosacral therapy for the damages caused by just this one practitioner.
Craniosacral therapy is based on a theory that lacks any plausibility, and there is no evidence either of the treatment being safe or effective.
Therefore we think that craniosacral treatment for infants is inherently dangerous.
There is no evidence whatsoever that there are any benefits to craniosacral therapy, except for curing fat wallet disease. Because of that, the risks of craniosacral therapy outweigh the benefits, by definition.
Yes, doctors do make mistakes. Sometimes terrible ones. That is extremely painful and sad for the victims. But: since medicine has started to embrace the scientific method, a hundred years ago, it has steadily improved and managed to all but double the average life span. Unless you think that living longer, happier, richer, healthier lives is a Bad Thing, you will have to admit that we made a good deal. A good deal that can be made even better by improving further.
In comparison to the wishful thinking of the craniosacralists, this is a wonderful record.
Indeed it is. 🙂
In reaction to this article, the “Nederlandse Cranio Sacraal Vereniging” (Dutch CranioSacral Association) said they do not recognise this manipulation. But the treatment in question was performed by a certified craniosacral therapist. What are parents to do – check all the study material before they visit a therapist?
I don’t see how not to make the connection between living happily for 3 months, then going to a therapist and having something done from which I turn blue and stool within 2 minutes, then die within 12 hours. Just don’t.
The article says “manipulations” and “continued and deep bending of the neck” which no CST system I know of practices. Are you sure that the therapist was a member in good standing with a recognizable CST training curriculum, or just using the title while practicing high velocity manipulations (which should never be done on children, let alone adults)
What were the credentials of this individual?
The therapist was an officially trained Upledger craniosacral therapist. The practice where he was employed gives craniosacral therapy according to the principles of John Upledger.
I’m an osteopathic medical student, so I feel compelled to chime in on this tragedy in a possibly unexpected manner. I’m constantly surrounded by purveyors of alternative treatment (thank god the scientific part of my education is isolated from these wack jobs), and I’ve got to say, I’ve been open minded in the past, but have basically come to the conclusion that basically anything labeled alternative medicine is bullshit. Most of it isn’t harmful beyond emptying the wallets of the gullable (which, i guess, is pretty damn harmful). But manipulation of the spine and hea, IMO, should never ever ever be done. It’s been done to me. There are risks, and no evidence beyond that which would be considered anecdotal (like drinking water upside down eliminates hiccups). Anyway, beware of non-mainstrean medicine. Although a lot of medicine is profit driven (big pharm, etc.), and sometimes shady science takes place to make the cash role in, there is disproportionately enormous fear of drugs and mainstream medical care that needs to lighten up. The FDA is the good guy. The NIH is the good guy. Egos, profits, and mistakes are a part of everything. Medicine should be evidence based. After all, any good decision in life is.
Dear Eric,,,yours are the last to read..after I paged through many other of the comments…I work in both the medical and “alternative” fields…and find all the scientific descriptions and comments honestly interesting…and my mind and intellect rushing…In the end…I have four children…of which two twins…and I followed strictly the medical model for the first two and even the third…until I got fed up with scientific egotistical medical practitioners…havin tenfolds of invasive test done on my kids…and all the results leading to NO answer….no real conclusions…until I face a colleague and asked him if he could believe that the tests results could possible be all correct and I have to take my sick child home and forget about it….how many tests…how many wrong treatments…chemically indused…AND SORRY TO SAY…THAT IS OKAY….CHEMICALLY INDUCED MEDICAL FAILURE OR LOSS OF LIFE…..WHAT DO WE CALL THAT…..I won’t even go there…polypharmacy in the search for an answer to something which might be as simple as an invasive birth process….
Point here…THE HUMAN BODY WAS DESIGNED AND MADE TO FUNCTION OPTIMALLY IF ALL GOES ACCORDING THE WAY NATURE MADE IT…BUT……………THAT SAID….NATURE IS NOT WHAT WE ALL GO BY…FOR SURE …I WOULD NOT HAVE HAD ANY OF MY KIDS IF I ALLOWED MIDDLE AGE NATURAL BELIEFS TO PICK FOR ME…SO THANK GOD FOR MEDICINE…BUT…. there is a beautiful bridge between medicine, science for some…..and natural healing, exquisite science for me….
Never should one modality claim king and master over the other…
The human body is so itricate and interesting..the human mind…those two cell getting together…with ALL the intelligence to form a perfet human body…on biological and cellular level…and where does the life sprint from….only those cell as hard science…or also intelligent messages…okay I am getting deep here…but my child was cramped in the uterus…c section birth….and his skull was totally out of shape…he cried 24/ 7 for 8 months…and stayed very much this way till almost 5 years…and I was too scared to move outside my field of knowledge ( which was then all clinical medicine…and law studies…) …pregnant with the next child…the 5year old begged me to help him…and I started trusting more than chemicals…and it worked….
Unfortunately damage has been done by medicine…and I waited tooooo long…but dedication and good combination of medicine,, complimentary and Godgiven Healing Hands…logical thinking and acceptance of more than one form of healing intelligence freed my child from lots of symptoms…and delivered a free person to the world.
Parents just want what is good and best for their kids…they seek help , these parents came to a therapist…as I went to a doctor…my child’s meningitis…haha…let’s not go there…or shall we…induced by so many factors which was propagated by the medical world….mercury poisoning…He could have died….but he did not…MEDICINE and a Paediatrician pulled him through…
What I am saying …is…STOP
Let the blind not call the weaksighted names, and vice versa…
I became also a craniosacral therapist…still in the medical fields too…and studied the phsychology of the books…and the human ….MRI scans..CT scan…ultrasound…and still
What is it that calms a baby…The first ever Craniosacral Therapist …a mother or a carers loving hands…LOOK….CAN YOU SEE….?????????????????
She is HOLDING him….against her chest…shoulder…her one hand cradled in the neck…the other over the little childs sacrum…and a calmness comes over the infant…THAT is a form , the very most special form of CST…combined with safety, care etc.
True non invasive CST …should never include overstretching…over bending…and not LISTENING to the signs….
I am truly sorry for these parents who took a baby to benefit optimally…and they lost their child…
I am sorry for the damage done to the profession which is there to help…
R M
@Jordana
Well, apparently it does. Bending an infant in the way the therapist did, even with minimal force, is extremely dangerous because the baby very easily is manipulated into a position in which it cannot breathe. The same thing can happen with babies in a sling, hence the warning issued by the US government.
What happened was that an infant was killed by quack treatment administered by a quack.There’s no excuse for that and in my opinion these things should be illegal.
There even are craniosacral therapists who claim their treatment can be used to treat cancer. *sigh*
I guess this is not the place and medium to be degrading about a career which is clearly not for everyone.
How many mistakes by other professionals are being burried….? I just wonder.
I believe it is good to have insight and also have some light on issues as the above…for bringing matters of concern under all professionals’ attention and also to keep the standard of practice up. But to call this a quak treatment is not just degrading it proofs that the above comment comes from a person who is probably not ready and willing to invest enough research into a field which brings so much relief where others gave up.
*sigh*
I’m sorry, but I think there is no scientific evidence cranioscral therapy works. Besides, the skullbones in an adult are grown together, so they can’t be moved. It’s not the single fact things can go horribly wrong, but also that there has never been proven a real positif effect.
@Rita
This was not a mistake, it was far worse than a “mistake”; it was the outcome of a therapy that not only is completely unproven but also based on nonsensical principles, performed by a therapist who had no idea that what he was doing could kill an infant and why. That is quackery, plain and simple. It has nothing to do with a “mistake”, honest or otherwise.
you have simply not read enough, researched enough >>> one simple point…logical…the cranial sutures…are BUT DEFINITELY NOT LOCKED AND UNMOVEABLE…. it is tongue and groove suture….the skull itself developed from ossification centres in the Dura Mater….did it ever divide…DEFINITELY NOT…. please…be welcome and do intensive research and not only clinical medical negativity.
The changes this therapy has brought to many people is amazing…consider the positive side too.
It certainly looks like they are on this photo.
God forbid the cranial bones should not be solidly joined, I’m very glad they are.
What use is a discussion with someone who flatly denies a reality that is observable to everyone?
Perhaps Rita should read this:
http://www.sciencebasedmedicine.org/index.php/alas-poor-craniosacral/
@Renate
Indeed she should, and this in particular:
I’ve been reading the commentary here and I see problems with people hearing what the other one is saying. To me the issue is the child died at the hands of a person who said they were trained in CST. Practitioners of CST have been saying: the maneuver he/she used was not a part of what is legitimate CST treatment practice, cut something else entirely. I see it in the same light of an intern, who is legitimately capable of much medical practice performing brain surgery, after which the patient died. S/He was performing a manipulation which is outside his/her scope of legitimate practice and which cannot be called intern level of competence. It was not a Cranial Sacral maneuver that was used on the deceased child as I understand Upledger Cranial Sacral Procedure. ( I will mention that I am an LMT and a Licensed Massage Therapy Instructor with several university degrees to my credit and that I have taken courses in CST from Upledger and others.) Gentle, slow, nurturing . . . relaxing. I can hold responsible a practitioner claiming certain skill levels and training for performing maneuvers which are not within his/her scope of practice. But the baby should not be tossed with the bathwater. The maneuver you are all blaming for the death of the baby is not the purview of CST as the CSTs I know practice, nor have I ever seen it in the literature or texts with which I am familiar.
@Greycat1
The person didn’t just say he was trained in CST as you put it; he was trained in CST: he was a certified John Upledger CS practitioner in a practice that specializes in John Upledger craniosacral therapy.
I don’t really care whether this was or was not the “purview of CST”, as CST, whatever it may or may not comprise, has no basis in reality to begin with: it is complete and utter nonsense. And when people are “taught” one kind of nonsense, there’s no knowing what other nonsense they may believe or fantasize, because in CST, as in all quackery, there are no reality checks, which means that anything goes.
A good idea. And that is exactly what a group of Canadian researchers did making this systematic review.
They did an extensive search for data. In section 2.3 sources of information (in addition to databases covering traditional medical literature) are mentioned:
And still the conclusion was:
Pingback: Craniosacral Therapy: Pure, Unadulterated Quackery - Skeptical Health : Skeptical Health
As a craniosacral therapist trained and working in Australia I would like to say that I have never seen or heard of a forced bending or manipulation as described in this article. It is not a CST technique. As all the other therapists have stated, CST is very gentle with no forced manipulations, in fact manipulation us a word never even used in the practice! Who knows where the therapist in question learnt it? Many Cranio therapists are also trained in other modalities, so perhaps it is
some other technique he had used???It is very sad that a child has died because of careless practice that remains unknown.
Pingback: Cranio Sacral Therapy
I just had this done yesterday, and it was very gentle. My neck was not forced in any direction – my neck went where it wanted to go! It is very sad however to hear of an infant death – regardless of the cause.
I got CST from a lady. She pressed neck area and I thought she pulled my neck. After I got the therapy, I had headache, felt dizzy, low energy, backache, and chest pain. After two weeks I am still struggling. I do not recommend anyone to take a risk. I hope I can recover from it.
Many of these comments are along the lines of “no true Scotsman”.
After a treatment during a cranio course i got sick.Instead of sending me to a professional i was give rescue drops.(very unprofessional in my eyes)I was ill for 7 years!
I reported later the incident to the cranio sacral association in the UK..That is the final replay of the chairman in original words.:
“Over the years i have come to realize that it is possible for someone doing this work to do real harm.How and why I do not know but it seems to be something destructive or negative or unblanced in the mind of the of the practitioner.I emphasise that I do not know if this was true of….(name).
Hopefully it is rare,but no one really knows.Of course those who do believe craniosacral is just imagination and placebo could never accept this.As they do not believe there is any good result,they can hardly believe in bad results.Perhaps one day somebody will find a way of researching this.It is very troubling but how can we find out the truth in this matter”
I think this statement is more than troubling.
I searched the net for a while and found out that nearly every Craniosacral Therapist has a esoterc background from Schamanism , over Reiki and all that stuff and no proper medical training.Many are medical laymen or bored house wives.
Under this aspect the so popular resolution of birth trauma,especially for babies, is irresponsible in my eyes.
Furthermore, nature has arranged things in such way that birth is traumatic AND that we have no recollection of it.
@ Ravi Singh
I think you are right. Many of the comments certainly resemble what we see in the “No true scotsman” fallacy. Proponents/practitioners of CST certainly claim that the practitioners of CST where things went wrong didn’t practice true CST.
As a side note it is interesting that what a “true CST practitioner” does, will not work through the mechanism it is supposed to.
Nice try!!
I like your no true scotsman page.But,
after i reported and complaint about the unprofessional treatment i had a hacker in my gmail from the UK.I had opened this account only for this reason and it was the only e mail at the time in this account.This shows me the criminal energy of the person and that me complaint was justified.
And i am a firm believer , medical laymen should not play with the central nervous system.
I absolutely agree.
I am not sure if you misunderstood my comment about the no true scotsman fallacy. If you read the comments made by craniosacral therapists who commented this post, you will find that they claim that the type of craniosacreal therapy you and other people were given by certified craniosacral therapists was not true craniosacral therapy. No matter what they say – you were told by a craniosacral therapist, that you were given craniosacral therapy – just as the (true) scotsman Lachlan put sugar on his porridge.
Who are “real craniosacral therapists”This was an instructor and i was attending a training.
He is still happily practicing under the protection of the UK association.
I watched the you tube videos
about babies…They all are crying and you can see how uncomfortable they are.There might be a few serious Ostheopaths around,they have at least a better training.But even among them you find all these”healers” floating around overestimating themselfes,charging a lot of money for fooling patients.Many Craniosacral therapists proclaim to treat Trauma.None of them is skilled to deal
physicly and psychologicly with a triggered Trauma.
Number 1: please leave chiropractors out of this. In my education anything resembling an adjustment to a child can only be done after the age of 7 years. Before this time the adjustments are soft touch and very comfortable involving NO rotation of the neck.
Number 2: who was this person? What were the credentials ? Are Cranial Sacral therapists doctors ? And if they are not doctors, then why are they treating patients? Regardless, the pediatrician should always be consulted before infants undergo any kind of therapy.